Long-term Watchman Data Reassure: CAP and CAP2 Registries
Experts say the field is maturing, with registries filling in the gaps about long-term safety of LAA occlusion for stroke prevention.
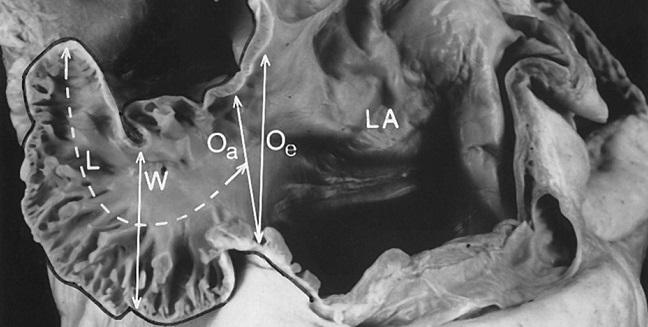
Long-term follow-up data from the continued access registries for the Watchman (Boston Scientific) left atrial appendage (LAA) closure device suggest that while it is being implanted into sicker and higher-risk patients than those included in the randomized trials, safety and efficacy are on par with, or better than, those earlier studies.
The rate of hemorrhagic stroke “is the lowest reported” to date, say investigators, with 0.17 and 0.09 events occurring per 100 patient-years in the Continued Access to PROTECT-AF (CAP) and Continued Access to PREVAIL (CAP2) registries, respectively. When the observed rate of ischemic stroke was compared with the predicted rate based on the cCHA2DS2-VAS scores, the Watchman device reduced the relative risk of ischemic stroke by 78% in CAP and by 69% in CAP2.
“With a device in place, it becomes part of the [patient’s] landscape, so longer pieces of information are incredibly important,” David R. Holmes Jr, MD (Mayo Clinic, Rochester, MN), who led the registry analysis, told TCTMD. Patients in CAP and CAP2 differed slightly, with the latter being older and at a higher risk for stroke, but the registry results are consistent with the randomized trials, he added.
In the field, it will be an ‘either-or.’ That would be the goal. David Holmes
“The future of the field is such that when patients come in with atrial fibrillation we’ll be able to have an upfront conversation with them where, if they’re at risk for stroke, we have in this setting two different treatment options,” said Holmes. “They both give good results. You can choose a device, which has the characteristics of the Watchman device. Most of the time you won’t need an anticoagulant and you’re going to have a marked reduction in hemorrhagic stroke.”
Other patients, he said, won’t want to take any chances with a procedure for stroke prevention and will instead opt for oral anticoagulation knowing they can fill a prescription that afternoon. “In the field, it will be an ‘either-or,’” Holmes said, referring to LAA occlusion devices or medical therapy. “That would be the goal.”
Andrew Goldsweig, MD (University of Nebraska Medical Center, Omaha), who was not involved in the analysis, said that in the field of structural interventions, LAA closure for stroke prevention is still in its infancy compared with TAVR and mitral valve procedures.
“We don’t have long-term safety and efficacy data,” he told TCTMD. “This is exciting especially as left atrial appendage closure matures and is offered to lower-risk patients with longer life expectancies. We need to know does this thing work in the long term. At this point, it’s been 10 years since the publication of PROTECT-AF and 5 years since the publication of PREVAIL, so this is big.”
Like Holmes, Goldsweig said the follow-up CAP/CAP2 registry data “move us one step closer to actualizing the shared dream of cardiologists everywhere who manage atrial fibrillation.” Because oral anticoagulation is poorly tolerated by so many patients and prescribed to less than half of those with atrial fibrillation, the emergence of an evidence-based, permanent alternative is a welcome treatment option, he said.
CAP and CAP2 Over the Years
The PROTECT-AF and PREVAIL studies, published in 2009 and 2014, respectively, showed that LAA closure with the Watchman device was noninferior to warfarin for preventing stroke and systemic embolism but superior in terms of preventing bleeding, including intracranial hemorrhage.
Watchman was approved by the US Food and Drug Administration in 2015 as an alternative to warfarin for stroke prevention in patients with nonvalvular atrial fibrillation, although the approval was a drawn-out process requiring multiple meetings with FDA advisory committees. The two registries were designed to allow continued patient access to Watchman prior to the US approval and to accumulate more data about the long-term safety and efficacy.
The CAP and CAP2 registries included 566 and 578 patients, respectively, who met the inclusion/exclusion criteria of the PROTECT-AF and PREVAIL randomized trials. Follow-up averaged at just longer than 50 months.
The primary and secondary endpoints in the CAP registry were identical to the study, while CAP2 used two primary efficacy endpoints and one safety endpoint consistent with PREVAIL. With CAP2, investigators used a second primary endpoint to evaluate the risk of ischemic stroke and systemic embolism within 7 days of the procedure as well as a modified safety endpoint to capture adverse events within the first 7 days.
This is exciting especially as left atrial appendage closure matures and is offered to lower-risk patients with longer life expectancies. Andrew Goldsweig
Patients in CAP2 were significantly older, including a larger percentage of above age 75, and had higher mean cCHA2DS2-VAS scores than those in CAP (4.5 vs 3.9; P < 0.0001). While they had a lower risk of bleeding, those in CAP2 were more likely to have hypertension, congestive heart failure, and diabetes.
In CAP, the primary efficacy endpoint—a composite that included stroke (ischemic and hemorrhagic), cardiovascular death (including unexplained death), and systemic embolism—occurred in 70 patients for a rate of 3.05 per 100 patient-years. In CAP2, the primary efficacy endpoint, which was the same as in CAP, occurred in 102 patients for a rate of 4.80 per 100 patient-years. In CAP2, the rate of ischemic stroke and pulmonary embolism was 2.2 per 100 patient-years. The most common event occurring during follow-up in both CAP and CAP2 was cardiovascular/unexplained death.
“It’s very positive in that the stroke rate is incredibly low and it doesn’t seem to get worse over the course of follow-up,” said Holmes. Complication rates, he added, were lower than in the randomized trials and oral anticoagulation was stopped in 95% of Watchman-treated patients at 1 year. “That was also seen in the randomized trials, but now we can see in this higher-risk group the [device] is still effective when you stop the anticoagulation,” said Holmes.
Watchman Outcomes: Rate per 100-Patient Years (95% Ci)
|
|
CAP |
CAP2 |
|
Primary Efficacy |
3.05 (2.4-3.9) |
4.80 (4.0-5.8) |
|
All Stroke |
1.48 (1.1-2.1) |
2.25 (1.7-2.9) |
|
Ischemic Stroke |
1.30 (0.9-1.9) |
2.20 (1.7-2.9) |
|
Hemorrhagic Stroke |
0.17 (0.06-0.5) |
0.09 (0.0-0.3) |
|
Systemic Embolism |
0.04 (0.01-0.3) |
0.09 (0.0-0.3) |
|
Cardiovascular/Unexplained Mortality |
1.69 (1.2-2.3) |
2.92 (2.3-3.7) |
|
All-Cause Mortality |
4.27 (3.5-5.2) |
6.24 (5.3-7.3) |
In CAP, which had a predefined safety outcome that included life-threatening events such as device embolization requiring retrieval, intracranial hemorrhage, gastrointestinal hemorrhage, and any bleeding related to the device or procedure, there were 66 adverse events (3.05 per 100 patient years). The most frequent adverse event was gastrointestinal bleeding (33), and half of these bleeds occurred within the first 45 days. In CAP and CAP2 combined, stroke related to device thrombus occurred in six patients while serious adverse events related to thrombus occurred in 16 patients.
When compared with outcomes in the randomized trials, the comparison that accounted for baseline CHA2DS2-VASc score showed that the primary efficacy endpoint, as well as cardiovascular/unexplained mortality, was not significantly different in the CAP/CAP2 registries than in PROTECT-AF and PREVAIL.
Registry Data vs Randomized Trials
In an editorial, A. John Camm, MD (St George’s University, London, England), states that LAA closure devices “offer a lifeline” to patients unable to tolerate oral anticoagulation, but adds that their value remains controversial. He calls for more research, particularly studies of LAA closure against direct oral anticoagulants (DOACs), studies of LAA closure in settings with reduced postprocedural antithrombotic therapy, and studies in patients unable to tolerate oral anticoagulation at all. While many of these studies have begun, enrollment is likely to be slow because “clinical equipoise is just about lost,” particularly for physicians who have already been using LAA closure devices in these settings, writes Camm.
Overall, the CAP/CAP2 registry data are helpful in that they provide more information about device safety, he says, but the efficacy data, particularly the predicted reduction in ischemic stroke that is based on the cCHA2DS2-VAS score in untreated patients, are more difficult to appraise.
“Despite the accumulation of very substantial registry data, guideline writers will understandably remain cautious about their recommendations for use of LAA closure implantation as an alternative to oral anticoagulation, but it is increasingly clear that, for those who have no alternative because they cannot take long-term oral anticoagulation, this therapy is well worthwhile,” according to Camm.
Holmes acknowledged the continued debate in cardiology about information gleaned from registries versus data obtained from randomized trials. “In some aspects,” he said, “they’re a matched pair. Randomized controlled trials tell us what to do in an ideal world, but we don’t live in an ideal world.”
Goldsweig added that the trials Camm calls for are either underway or have been conducted. For example, the PRAGUE-17 trial, which was presented at the European Society of Cardiology 2019 Congress, showed that LAA occlusion with the Amplatzer Amulet (Abbott) or Watchman devices was noninferior to more contemporary DOAC therapy. The ongoing ASAP-TOO trial, for which Goldsweig is an investigator, is currently testing LAA closure in patients unable to tolerate oral anticoagulation.
While CAP and CAP2 included only 1,100 nonrandomized patients, Goldsweig said a lot of data in structural heart disease are derived from registries because of the high costs of the device and procedure.
“Really, the only randomized trials you’re going to get are going to be industry sponsored,” he said. “No institution can afford significant randomized trials so we’re left making do with registry data. In the United States, the FDA has made that much easier because they require everybody to participate in the [American College of Cardiology’s National Cardiovascular Data Registry LAAO Registry], which, at this point, includes about 90,000 patients. The first analyses are already underway, and I think they’ll be able to powerfully confirm these findings and generate a lot more knowledge about LAA closure.”
Photo Credit: Kar S. Watchman I: device evolution, patient selection, and tips and tricks. Presented at: TVT 2019. June 13, 2019. Chicago, IL.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Holmes DR, Reddy VY, Gordon NT, et al. Long-term safety and efficacy in continued access left atrial appendage closure registries. J Am Coll Cardiol. 2019; 74:2878-2889.
Camm AJ. Do data derived from registries help or confuse the assessment of left atrial appendage closure? J Am Coll Cardiol. 2019; 74:2890-2892.
Disclosures
- Holmes reports serving as a member of an advisory board (unreimbursed) for Boston Scientific.
- Camm reports receiving institutional grants and personal fees from Bayer, Boehringer Ingelheim, BMS/Pfizer, and Daiichi-Sankyo. He reports receiving personal fees from Abbott, Boston Scientific, and Medtronic.


Comments