Postoperative AF ‘Not Benign,’ Just As Likely to Cause Stroke
Perhaps clinicians should consider a broader strategy for starting anticoagulation following noncardiac surgery, experts say.
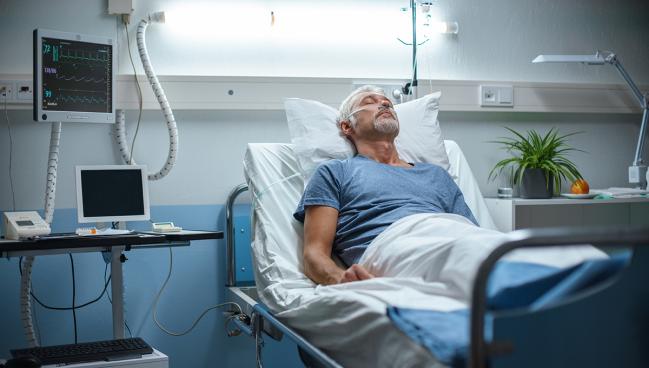
Patients who develop atrial fibrillation (AF) after noncardiac surgery are at a similar risk of thromboembolic events as those who develop AF in other settings, according to new observational cohort data.
The findings underscore the notion that postoperative AF “should not be considered a transient, benign phenomenon,” lead author Konstantinos C. Siontis, MD (Mayo Clinic, Rochester, MN), and colleagues write. “Rather, it is an arrhythmia that seems to portend similar thromboembolic risks as AF diagnosed outside of the operative setting.”
To TCTMD, Siontis characterized postoperative A-fib after noncardiac surgery as “almost like an orphan disease in the sense that we've seen this and clinicians have dealt with it for many, many, many years but it has been somewhat ignored from the research and investigation standpoint up until recently.” Traditionally, he said, “it has been considered by clinicians as something that should come and go and not come back.”
The study, published online ahead of print this week in the Annals of Internal Medicine, confirms similar findings from a 2018 Danish study of administrative claims data. However, the authors claim their results, even though they’re derived from slightly less-contemporary data from 2000 to 2013, are strengthened by including “manual validation of all AF diagnoses and outcome events rather than reliance on diagnostic codes alone.” Another earlier study showed a link between postoperative AF and a higher risk of hospitalization for heart failure.
Similar Thromboembolic Risk
For the current study, the investigators included 4,231 patients with incident AF from their institution and Olmsted Medical Center; 13% had postoperative AF as their first-ever documented presentation. Mean age was about 73 years and just over half were male. Notably, more than 96% of the cohort was white.
Over 6.3 years of follow up, 11.5% had an ischemic stroke or TIA, 58.2% had a subsequent episode of AF, and 60.6% died.
In a weighted analysis, the risk of stroke or TIA was no different between those whose AF appeared after surgery and those who presented outside of the surgical setting (adjusted HR 1.01; 95% CI 0.77-1.32). There were also no differences in the risks of cardiovascular and all-cause death. However, patients with postoperative AF had a 13.4% lower risk of recurrent AF (adjusted HR 0.68; 95% CI 0.60-0.77).
Interestingly, the authors note that “half of the anticoagulant-eligible patients with postoperative AF never received an anticoagulant prescription.”
To TCTMD, senior author Alanna M. Chamberlain, PhD (Mayo Clinic), acknowledged that the data might not reflect current prescribing patterns and that the researchers did not have access to information on patient bleeding risk, which may have affected their medications. Still, she said, the fact that patients with postoperative AF “have a similar risk of stroke and death compared to other patients who develop atrial fibrillation unrelated to a surgery . . . should influence decisions on whether or not these patients should be anticoagulated.”
Siontis blamed the hesitation to prescribe anticoagulation to postoperative patients on the fear of additional risk of surgical-related bleeding.
“The bigger question that is still an unknown is: should we treat people who have postoperative A-Fib with anticoagulation even from the get-go?” he said, acknowledging that randomized data are needed to give proper guidance. “But I do think that we provide some justifications to at least think about anticoagulation in patients who are felt to be low risk for bleeding in the postoperative setting, and, at a minimum, allowing the patient to recover from surgery and then considering whether or not anticoagulation might be a good idea for them.”
Because most physicians don’t follow-up with ambulatory monitoring in patients with postoperative AF, Siontis guessed that if this was done more systematically, “we will see quite a bit of A-fib.” Ongoing prospective research, including a study of his own, should help to assess the incidence of subsequent AF, he said.
‘Mounting Body of Evidence’
Nishaki Mehta, MD (Beaumont Hospital, Royal Oak, MI, and University of Virginia, Charlottesville), who wasn’t involved in the study, said there is “a mounting body of evidence that we should not disregard postoperative atrial fibrillation. It may not be a one-off event.”
She agreed that there are likely multiple actors at play for why the condition hasn’t been taken as seriously as it should be by clinicians. “Now, I think we understand it could be the first manifestation of an underlying vulnerability that predisposes patients to A-fib,” Mehta told TCTMD, adding that increasing monitoring, especially with wearable devices, is picking up more of these arrhythmias.
In her clinic, she recommends that patients with postoperative AF “set up at least one visit with an electrophysiologist and follow up.” At that point, the clinician should explain that because the AF happened once, there’s a higher likelihood of recurrence, and ask how the patient would like to proceed. “Essentially, education is a big part of telling them that this could come back,” Mehta said.
“The second thing, which the authors noted [and] is not surprising, but I'm glad it's out there, is a lot of these folks were not prescribed anticoagulation because it was thought to be a one-off event,” she continued. “I really think the anticoagulation strategy should be guided more by the CHA2DS2-VASc scoring system. If that score is elevated, my philosophy is you can't go wrong by starting someone on anticoagulation and then as an outpatient discussing if you'd like to continue on long-term [treatment] or consider an interruptive strategy.”
In the future, Mehta said she would like to see a greater focus on “trying to determine early intervention for targeting the subsequent atrial fibrillation and preventing atrial myopathy. We've been studying this quite extensively in ‘bread-and-butter’ atrial fibrillation, but given that 13% of A-fib is postoperative, focusing on figuring out the role of early rhythm control would really guide us.”
Siontis would also like to see randomized, multicenter trials include a variety of patients and surgeries. “The majority of patients in our group had orthopedic surgeries, but there's a lot of other surgeries that could be associated with postoperative A-fib,” he said. “So it's important to carefully select types of surgeries, types of practices in community versus academic practices, [and] diverse patient populations racially and [in terms of] resource availability and follow-up healthcare utilization.”
Yael L. Maxwell is Senior Medical Journalist for TCTMD and Section Editor of TCTMD's Fellows Forum. She served as the inaugural…
Read Full BioSources
Siontis KC, Gersh BJ, Weston SA, et al. Associations of atrial fibrillation after noncardiac surgery with stroke, subsequent arrhythmia, and death: a cohort study. Ann Intern Med. 2022;Epub ahead of print.
Disclosures
- The study was funded by the National Institute on Aging.
- Siontis, Chamberlain, and Mehta report no relevant conflicts of interest.




Comments