Risk of Repeat Stroke Underrecognized in Nonstenotic Carotid Lesions
The CAPIAS trial suggests that substenotic plaque on MRI may play more of a role in ischemic stroke than previously thought.
Patients without obstructive stenosis in whom complicated carotid plaques are detected on MRI in the early days after an ischemic stroke or TIA are at increased risk for a recurrent cerebrovascular event, according to results of the Carotid Plaque Imaging in Acute Stroke (CAPIAS) study.
Those with the combination of cryptogenic stroke and ipsilateral complicated carotid plaques had the greatest increased risk of a repeat event in the study, with a 5.6-fold increased risk compared with patients who did not have complicated carotid plaques.
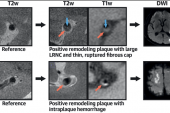
“We further found the presence of an ipsilateral ruptured fibrous cap and of intraplaque hemorrhage to be significantly associated with recurrent ischemic stroke or TIA,” write Anna Kopczak, MD (University Hospital, LMU Munich, Germany), and colleagues. They add that intraplaque hemorrhage can be reliably detected by MRI, suggesting that imaging for it could be integrated into the diagnostic workflow of anterior circulation stroke. The study was presented earlier this week at the European Stroke Organisation Conference and simultaneously published in the Journal of the American College of Cardiology.
Commenting on the study for TCTMD, Debabrata Mukherjee, MD (Texas Tech University Health Sciences Center, El Paso), said it extends the understanding of the relationship between these plaque features and recurrence risk to a population who would not normally be offered revascularization because their burden of stenosis is lower than what is considered a recognized risk for stroke. All patients in CAPIAS had carotid stenosis < 70%.
That being said, Mukherjee noted that without knowing how to change care for this group of patients, the results are at best hypothesis-generating.
“To me, the biggest question is :what do we do different?” Mukherjee said. “This is an interesting mechanistic study, but they need to take it to a larger patient population and figure out what, if anything, can be done to change how these patients are treated based on the data.”
Kopczak and colleagues acknowledge uncertainty about whether patients with cryptogenic stroke who have ipsilateral intraplaque hemorrhage or other complicated carotid plaques features would benefit from more-intensive medical therapy or carotid interventions. They also noted that treatment options for cryptogenic stroke are limited and that several trials of patients with embolic stroke of undetermined source (ESUS), including NAVIGATE-ESUS and RE-SPECT ESUS, have shown no benefits with anticoagulant therapy over aspirin.
The CAPIAS Trial
For the study, Kopczak and colleagues enrolled 196 patients from four tertiary care centers in Germany who had undergone carotid MRI within 10 days of a cryptogenic (n = 104), cardioembolic (n = 54), large-artery (n = 19), or small-vessel stroke (n = 19). At baseline, 29% of patients had ipsilateral complicated carotid artery plaques on imaging.
Over a mean follow-up of 30 months, 21 patients experienced the combined primary endpoint of recurrent ischemic stroke (n = 16) or TIA (n = 5). More than 50% of those who experienced a recurrent event had a cryptogenic first stroke. Among index cryptogenic stroke patients with ipsilateral complicated carotid artery plaques, the incidence rate of recurrent ischemic stroke or TIA over the follow-up period was 10.92 per 100 patient-years versus 1.82 per 100 patient-years for those without ipsilateral complicated carotid artery plaques (log-rank P = 0.003).
After adjusting for age and sex, having ipsilateral complicated carotid artery plaques was associated with significantly increased risk of a recurrence (P = 0.013). The results remained significant when the analysis was restricted to those with ipsilateral recurrent ischemic stroke or TIA (HR 5.01; 95% CI 1.25-20.05). Sensitivity analyses accounting for differences in stenosis grade and correcting for the presence/absence of contralateral complicated carotid artery plaques did not change the results in the overall cohort or in the subset of patients with cryptogenic stroke.
At 12-month follow-up, 107 patients underwent an additional MRI, with new brain lesions found in 35. Approximately half of those were definitive new ischemic lesions, with 12 classified as silent ischemic brain infarct. The remainder were preexisting small-vessel disease or unclear lesion type. Among the 107 patients, six experienced a recurrent ischemic stroke.
Next Steps, With Caution
“We envision the next step to be a multicenter study determining the precise prevalence of intraplaque hemorrhage and associated recurrence rates in unselected patients with anterior circulation stroke,” the researchers write. “Such a study would enable analyses in relevant subgroups in order to prepare for future prevention trials.”
Mukherjee said while further research is warranted, he would prefer to see an alternative imaging option, perhaps utilizing an ultrasound technique that would be less expensive than the MRI the researchers used, which had dedicated carotid coils. He also expressed concerns about putting recent stroke patients through a long imaging process with contrast.
In an editorial accompanying the study, Joshua Z. Willey, MD (Columbia University Irving Medical Center, New York, NY), and Gerard Pasterkamp, MD (University Medical Center Utrecht, the Netherlands), say the study raises important new suspicions about low-burden stenoses, which don’t fit into TOAST criteria for categorization of subtypes of ischemic stroke.
“The criteria for classifications in the context of atherosclerosis-related disease manifestations or lesion descriptions often originate from studies that were executed 20-30 years ago,” they write. Since that time, therapeutic strategies and survival rates have improved, lifestyle and smoking policies have changed, and the pathology of large-artery stroke may have shifted from ruptured to nonruptured plaques, Willey and Pasterkamp add.
“These changes indicate that the original data that underly the currently applied stroke risk classifications may not optimally apply to current times and merit careful consideration,” they say, adding that considering substenotic plaque in the context of ischemic stroke and recurrence, “broadens our understanding of the concept of ESUS.”
L.A. McKeown is a Senior Medical Journalist for TCTMD, the Section Editor of CV Team Forum, and Senior Medical…
Read Full BioSources
Kopczak A, Schindler A, Sepp D, et al. Complicated carotid artery plaques and risk of recurrent ischemic stroke or TIA. J Am Coll Cardiol. 2022;Epub ahead of print.
Willey JZ, Pasterkamp G. Vulnerable carotid plaque in cryptogenic stroke. J Am Coll Cardiol. 2022;Epub ahead of print.
Disclosures
- Kopczak, Willey, and Pasterkamp report no relevant conflicts of interest.


Comments