For Complex PCI, Intravascular Imaging Lowers Risk of TVF
The reduction in “hard” events in RENOVATE-COMPLEX-PCI caught some off-guard, but only bolsters calls for routine IVUS or OCT.
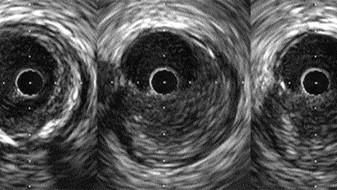
Photo Credit: Adapted from Mintz GS. What is essential to know about IVUS. Presented at: TCT 2022. Boston, MA.
NEW ORLEANS, LA—The use of intravascular imaging to guide complex PCI is associated with a significantly lower risk of target vessel failure when compared with conventional angiography, according to the results of the RENOVATE-COMPLEX-PCI study.
Senior investigator Joo-Yong Hahn, MD, PhD (Samsung Medical Center, Seoul, Korea), who presented the results during the late-breaking clinical trial session at the American College of Cardiology/World Congress of Cardiology (ACC/WCC) 2023 meeting, said the benefit of intravascular imaging was seen consistently across various types of complex coronary lesions.
While there is a large and growing body of evidence to support intravascular imaging for PCI, Hahn said cost remains a limiting factor with uptake. For that reason, they are currently performing a cost-effectiveness analysis in RENOVATE-COMPLEX-PCI, pointing out that only select cases will likely require imaging.
“I don’t claim that every procedure needs intravascular imaging,” he told TCTMD. “I hope that physicians and operators actively consider intravascular imaging for patients with complex coronary artery disease.”
Other operators at ACC/WCC these and other data clearly support the use of imaging over angiography-based PCI.
Wayne Batchelor, MD (Inova Heart and Vascular Institute, Falls Church, VA), chair of the ACC Interventional Council, said the debate is shifting towards “why not” as opposed to “why” when it comes to intravascular imaging. RENOVATE-COMPLEX-PCI, he said, “extends our previous knowledge about the incremental benefit of intravascular ultrasound or OCT and optimizing percutaneous coronary intervention results,” he said in a press conference. “To me, the intravascular ultrasound/OCT world has spoken. The only question is when is the interventional world going to listen?”
“The evidence is falling in place to support imaging-guided PCI,” interventional cardiologist Kevin Bainey, MD (Mazankowski Alberta Heart Institute/University of Alberta, Edmonton, Canada), told TCTMD. “It’s in that population of complex coronary artery disease where we’re now pulling out the OCT or high-definition IVUS to help us guide procedures. This study, I’m very impressed.”
Bainey pointed out that the trial included both stable ischemic heart disease and ACS patients.
“That imaging-guided PCI reduces death and MI, hard endpoints, that’s huge,” he said. “I think this will change people’s practice. There are costs attached to it, but this will push interventional cardiologists to say, ‘If we’re planning a complex PCI case, undoubtedly we should be using imaging guidance.’”
Also speaking with TCTMD, Sanjit Jolly, MD (McMaster University, Hamilton, Canada), said there is a groundswell of support for intravascular imaging based on prior IVUS data. In Ontario, the provincial government recently launched additional funding for PCI cases with intravascular imaging. As a result, hospitals will be more encouraged to use it. “From a practical viewpoint, a lot of imaging catheters have gone on back order because there is such increased use in Ontario,” he said.
Bigger Push for More Imaging
The American College of Cardiology, the American Heart Association, and the Society for Cardiovascular Angiography and Interventions (ACC/AHA/SCAI) guidelines for coronary revascularization recommend IVUS for procedural guidance, particularly in cases of left main or complex CAD. OCT is considered a reasonable alternative to IVUS for procedural guidance, according to the guidelines, except in ostial left main disease. Guidelines from the European Society of Cardiology and European Association for Cardio-Thoracic Surgery (ESC/EACTS) also recommend IVUS or OCT for selected patients to optimize stent implantation.
Just last month, the ACC Interventional Council took a strong stance on the use of intravascular imaging, stating that it should be a routine part of everyday practice. Specifically, intravascular imaging should be considered an “essential adjunct to angiography” for left main, proximal LAD, in-stent restenosis, stent thrombosis, calcified coronary arteries, and CTOs, or any other scenario where angiography fails to shed light on the coronary anatomy.
Despite the recommendations, uptake of intravascular imaging in the US lags behind other countries, particularly those in Europe and Asia. In one study from Michigan published last year, intravascular imaging was used in roughly 16% of PCIs, with investigators noting wide variability among physicians and centers. Use of imaging did appear to be on the rise, though.
In RENOVATE-COMPLEX-PCI, patients were randomized 2:1 to intravascular imaging with IVUS or OCT or to angiography-guided PCI. Patients were included in the study if they had a true bifurcation lesion, CTO, unprotected left main CAD, long coronary lesions (stent length at least 38 mm), multivessel CAD with at least two major epicardial coronary arteries, lesions requiring multiple stents, in-stent restenosis, severely calcified lesions, or ostial lesions of a major epicardial artery.
Patient characteristics, including the types of complex coronary lesions, were balanced between the two groups. The initial presentation was split equally between stable ischemic heart disease and ACS, with 18.2% of the ACS group presenting with an acute MI. Most patients randomized to intravascular imaging were treated using IVUS (73.3%) and the majority of cases were performed via the radial artery. Nearly 80% of patients randomized were male (mean age 65.6 years). The median procedural time was longer with intravascular imaging (70.0 versus 53.5 minutes).
At a median follow-up of 2.1 years, the primary endpoint—target-vessel failure, comprised of cardiac death, target-vessel MI, or clinically driven target-lesion revascularization—was reduced with intravascular imaging. Similarly, the secondary endpoint of target vessel-related MI or death from cardiac causes was 37% lower compared with angiography-guided PCI.
RENOVATE-COMPLEX-PCI Outcomes
|
|
Intravascular Imaging-Guided PCI (n = 1,092) |
Angiography-Guided PCI (n = 547) |
HR (95% CI) |
|
Primary Endpoint |
|||
|
Target-Vessel Failure (Cardiac Death, Target-Vessel MI, or Clinically Driven TLR) |
7.7% |
12.3% |
0.64 (0.45-0.89) |
|
Secondary Endpoints |
|||
|
Target-Vessel Failure Without Procedure-Related MI |
5.1% |
8.7% |
0.59 (0.39-0.90) |
|
Target Vessel-Related MI or Cardiac Death |
5.3% |
8.5% |
0.63 (0.42-0.93) |
|
Cardiac Death |
1.7% |
3.8% |
0.47 (0.24-0.93) |
|
Target Vessel-Related MI |
3.7% |
5.6% |
0.74 (0.45-1.22) |
|
Target-Vessel Revascularization |
3.4% |
5.5% |
0.69 (0.40-1.18) |
|
Target-Lesion revascularization |
2.6% |
4.4% |
0.66 (0.36-1.22) |
Intravascular imaging was also associated with a 53% lower risk of cardiac death, a finding that surprised some, including Roxana Mehran, MD (Icahn School of Medicine at Mount Sinai, New York), the scheduled discussant following the late-breaking clinical trial’s presentation. “A massive reduction in cardiac death,” she said. “That was striking to me.”
Jolly was also surprised by the reduction in cardiac death, saying that it should be considered hypothesis-generating at this point.
Hahn, for his part, believes the finding to be real, noting that this trial, as opposed to those that came before it, is larger, had longer follow-up, and included patients undergoing complex PCI. “That’s why our results differ from the previous trials,” he said.
In the ULTIMATE trial, which was conducted at eight centers in China, IVUS-guided PCI with DES resulted in significantly lower rates of target vessel failure at 1 year in an “all-comers” population, a benefit driven by a reduction in target-lesion revascularization. That reduction was maintained at 3 years. Additional trials, including IVUS-XPL, have also shown lower rates of various major adverse cardiovascular events with IVUS, said Hahn, but these trials included highly selected coronary lesions. Meta-analyses, including one published in 2020, showed that IVUS guidance was associated with lower risks of cardiovascular death, MI, target-lesion revascularization, and stent thrombosis compared with standard angiography-guided PCI.
“When you put all of the data together, you see somewhere in the range of a 40% to 50% reduction in target vessel revascularization with intravascular imaging,” said Jolly. “Of course, people still question that. IVUS use in the US is still quite low, certainly less than 20%.”
Full Expansion of Stent
In terms of why there was a reduction in hard clinical endpoints, operators point out that intravascular imaging allows them to plan and complete their procedures much better than with angiography alone.
“With intravascular imaging, we see what’s happening below the surface,” said Jolly. “We can plan the lesion length, the vessel diameter, and once we deploy the stent, we can optimize it in terms of expansion. Oftentimes things look pretty good on the angiogram and we’re about to finish, but then we do the intravascular imaging and realize there’s some underexpansion.”
Areas of underexpansion, he added, are segments susceptible to restenosis. “If you don’t optimize the stent, they can end up coming back,” he said.
One question that often comes up is why not just skip postprocedure intravascular imaging and perform adjunctive balloon dilation in all implanted stents to ensure sufficient stent expansion. The evidence suggests that strategy doesn’t work, said Jolly. “If you’re aggressively postdilating when you don’t need to, then you can run into problems of dissections and perforations.”
Bainey pointed out that the benefits of intravascular imaging were apparent quite soon after PCI, adding that the reduction in hard clinical events is likely derived from appropriate stent expansion with imaging. “With angiographic guidance, I think we’re notoriously underexpanding our stents,” he said. “With imaging guidance, it’s very clear whether or not you’re underexpanded. With OCT, it’s actually quite good—the software just spits the information out. There’s no question in my mind that it’s postexpansion.”
Batchelor said that clinical guidelines tend to be behind practice, but there is a greater push for regular use of IVUS or OCT for PCI, particularly in complex cases. The ACC Interventional Council, he said, is currently focused on physician education, noting they have hosted numerous webinars in addition to their recent evidence review.
Michael O’Riordan is the Managing Editor for TCTMD. He completed his undergraduate degrees at Queen’s University in Kingston, ON, and…
Read Full BioSources
Lee JM, Choi KH, Song YB, et al. Intravascular imaging-guided or angiography-guided complex PCI. N Engl J Med. 2023;Epub ahead of print.
Disclosures
- Hahn reports grant support from Abbott, Biosensors, Biotronik, Boston Scientific, Daiichi Sankyo, Donga-ST, Hanmi Pharmaceutical, Medtronic, and the National Evidence-based Healthcare Collaborating Agency.



Comments