COVID-19: TCTMD’s Daily Dispatch for July
We’re curating a list of COVID-19 research and other useful content, and updating it daily.

TCTMD reporter Todd Neale is keeping up on breaking news and peer-reviewed research related to COVID-19 and will update daily. If you have something to share, tell us. All of our COVID-19 coverage can be found on our COVID-19 Hub.
July 31, 2020
 A French analysis shows that elevated coronary artery calcium is a marker for worse prognosis among patients hospitalized for COVID-19, TCTMD’s Yael Maxwell reports. Although small, the study supports the practice of analyzing CAC in every COVID-19 patient, since it is a “freebie” that can help plan appropriate management, commented Harvey Hecht, MD. “You're getting a CT scan of the lungs on every COVID patient and that information is just there. You simply can't miss it. So it takes virtually no additional time to do the measurements.”
A French analysis shows that elevated coronary artery calcium is a marker for worse prognosis among patients hospitalized for COVID-19, TCTMD’s Yael Maxwell reports. Although small, the study supports the practice of analyzing CAC in every COVID-19 patient, since it is a “freebie” that can help plan appropriate management, commented Harvey Hecht, MD. “You're getting a CT scan of the lungs on every COVID patient and that information is just there. You simply can't miss it. So it takes virtually no additional time to do the measurements.”
A panel of experts give a weak recommendation for remdesivir (Gilead Sciences) for the treatment of severe COVID-19 in a “rapid recommendation” document published in the BMJ. They encourage continued enrollment of patients into randomized trials evaluating the drug. The guidance was based on a systematic review and network meta-analysis “showing low-certainty evidence that remdesivir may be effective in reducing time to clinical improvement and may decrease mortality in patients with severe COVID-19.”
 A German autopsy study suggests that at least some of the myocardial injury seen in COVID-19 patients may be related to active virus replicating in heart tissues—an issue of long-running debate with this disease. Though autopsy reports from COVID-19 have been limited, Gregg C. Fonarow, MD, told TCTMD’s L.A. McKeown, “they do give important insights for which there are clinical correlates.”
A German autopsy study suggests that at least some of the myocardial injury seen in COVID-19 patients may be related to active virus replicating in heart tissues—an issue of long-running debate with this disease. Though autopsy reports from COVID-19 have been limited, Gregg C. Fonarow, MD, told TCTMD’s L.A. McKeown, “they do give important insights for which there are clinical correlates.”
At one large academic medical center, a “detailed triage process using physician-level review to determine whether to perform, defer, or cancel inpatient transthoracic echocardiogram (TTE) requests based on indication and clinical urgency” selected TTEs for more critically ill patients and reduced the number of TTEs for patients with confirmed COVID-19 by 60%, according to data in the Journal of the American Society of Echocardiography. The process didn’t delay TTE for patients with pending COVID-19 tests or increase adverse cardiovascular outcomes.
In PNAS, researchers propose a strategy for initiating temporary shelter-in-place orders when local hospital admissions for COVID-19 exceed a specified threshold. Such an approach “can mitigate the impact on the community’s healthcare system while minimizing economic and societal costs,” they say.
 Another study in PNAS shows that how people respond in terms of social distancing to emergency declarations is dependent on income level. Using mobile device data, investigators found that “wealthy areas went from most mobile before the pandemic to least mobile, while, for multiple measures, the poorest areas went from least mobile to most.”
Another study in PNAS shows that how people respond in terms of social distancing to emergency declarations is dependent on income level. Using mobile device data, investigators found that “wealthy areas went from most mobile before the pandemic to least mobile, while, for multiple measures, the poorest areas went from least mobile to most.”
A JAMA viewpoint discusses what can be done to avoid Strongyloides hyperinfection or dissemination syndrome, a potentially severe but uncommon complication of treatment with dexamethasone, which has increased in use after showing efficacy in treating COVID-19. “Strongyloides hyperinfection syndrome is potentially catastrophic to patients. It is possible that as dexamethasone becomes more widely prescribed for individuals with COVID-19, a substantial number of patients may be at risk,” the authors note.
“Children younger than 5 years with mild-to-moderate COVID-19 have high amounts of SARS-CoV-2 viral RNA in their nasopharynx compared with older children and adults,” suggesting that young children may be important drivers of the spread of the virus, according to a study in JAMA Pediatrics. “Behavioral habits of young children and close quarters in school and day care settings raise concern for SARS-CoV-2 amplification in this population as public health restrictions are eased,” the authors say.
That finding, however, is somewhat at odds with a recent rapid review published by the National Collaborating Centre for Methods and Tools, in Canada, which concluded that young children are not a major source of COVID-19 transmission. “Analyses of infection clusters revealed that for children who were infected, transmission was traced back to community and home settings or adults, rather than amongst children within day cares or schools.”
"Buddy liked dog stuff: running through the sprinklers, going on long car rides, swimming in the lake. He cuddled the Mahoneys—his owners and family—at the end of tough days. He humored them when they dressed him up as a bunny for Halloween.” Buddy, the first dog to test positive for COVID-19 in the United States, died on July 11, National Geographic reports. He died 6 weeks after first developing shortness of breath.
Buddy, the first dog in the U.S. diagnosed with the coronavirus, has died. His family shared their frustrations and heartbreak with @natashaldaly https://t.co/jxDUNm8spv
— National Geographic (@NatGeo) July 30, 2020
July 30, 2020
 Around the United States, physicians across specialties have seen dramatic, sudden drops in patient volumes and revenues as elective procedures and testing ground to a halt and people isolated in their homes, and it’s been no different for cardiology. I spoke with cardiologists and practice administrators to get a sense of the financial impact of the pandemic and how the recovery is going. “What we have seen is very serious—just unbelievably serious—impacts in certain areas of the country from the healthcare effects of COVID, but what we’ve seen throughout the country is the economic carnage,” said Jerry Blackwell, MD, MBA, president and CEO of MedAxiom.
Around the United States, physicians across specialties have seen dramatic, sudden drops in patient volumes and revenues as elective procedures and testing ground to a halt and people isolated in their homes, and it’s been no different for cardiology. I spoke with cardiologists and practice administrators to get a sense of the financial impact of the pandemic and how the recovery is going. “What we have seen is very serious—just unbelievably serious—impacts in certain areas of the country from the healthcare effects of COVID, but what we’ve seen throughout the country is the economic carnage,” said Jerry Blackwell, MD, MBA, president and CEO of MedAxiom.
The United States has exceeded 150,000 COVID-19 deaths, shooting past previous projections from earlier in the year, the New York Times reports.
Tocilizumab (Actemra; Roche) does not look like it’s going to pan out as a treatment for patients hospitalized with severe COVID-19-related pneumonia. The phase III COVACTA trial failed to meet its primary endpoint of improved clinical status, showing also that the drug did not reduce mortality, Roche announced in a press release.
The more I see the less I understand and even @ProfDFrancis can't help. Was the patient in Figure 1 taking part in the study? Figure 1 says they had a Trop T of 17.8pg/mL 78 days after diagnosis. Can anyone show me the point on Figure 3(c) with x=78 and y=17.8? https://t.co/Zdvmtn9Xc9 pic.twitter.com/gI1cBgumfH
— Graham Cole (@drgrahamcole) July 29, 2020
Signs of cardiac damage are seen on CMR even in younger, nonhospitalized COVID-19 patients, according to a study in JAMA Cardiology. Despite the fact that 67% of the patients who volunteered for the study never required hospitalization, 78% had abnormal imaging findings 2 to 3 months after testing positive for the virus, TCTMD Managing Editor Shelley Wood reports. Commentators on Twitter raised some issues with the study.
In JACC: Case Reports, researchers provide details on two patients who presented with delayed STEMI and developed ventricular septal rupture. “The fear of contracting COVID-19 infection, although justified, will likely result in an increase in non-COVID morbidity and mortality caused by avoidance of the medical system,” they say.
An analysis of videos recorded in public in Asia, Western Europe, and the United States shows that mandates were associated with increased wearing of masks during the pandemic. In addition, researchers report in JAMA Network Open, mask wearing was tied to less face touching, which may reduce transmission risk.
Also in JAMA Network Open, a study shows that rates of deficiencies and complaints were higher in nursing homes that reported COVID-19 cases. “Nursing homes care for aging adults with chronic conditions and have experienced years of declining revenues and financial instability,” the authors write. “These factors have made many facilities ill prepared for a pandemic, and stemming the spread of COVID-19 in nursing homes will not be easy.”
Whether to open US schools in the fall—and how—is on everyone’s mind as the summer progresses. It’s the subject of two new articles in the New England Journal of Medicine—here and here—and a JAMA viewpoint describing a report on the subject from the National Academies of Sciences, Engineering, and Medicine.
 US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, spoke with Diana Bianchi, MD, director of the NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), about what is known about the effects of COVID-19 on child and maternal health. “I think parents should be generally reassuring to their children. We’ll get through this,” Bianchi said. “However, I would also say that if a parent notices something unusual going on with a child—skin rashes, the so-called blue COVID toes, or a prolonged fever—don’t mess around. Get your child medical attention as soon as possible. Bad things can happen very quickly to children infected with this virus.”
US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, spoke with Diana Bianchi, MD, director of the NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), about what is known about the effects of COVID-19 on child and maternal health. “I think parents should be generally reassuring to their children. We’ll get through this,” Bianchi said. “However, I would also say that if a parent notices something unusual going on with a child—skin rashes, the so-called blue COVID toes, or a prolonged fever—don’t mess around. Get your child medical attention as soon as possible. Bad things can happen very quickly to children infected with this virus.”
Also in JAMA, a study shows that school closures in the US reduced both the incidence of COVID-19 and related mortality, with greater gains in states that shut them down sooner. In an accompanying editorial, researchers write: “The decision to reopen schools for in-person educational instruction during the fall of 2020 is among the greatest challenges that the US has faced in generations. . . . There has rarely been a more important time for open discussion and collaboration with a goal of reaching consensus on reopening schools, while protecting the health and well-being of students and educators during the COVID-19 pandemic.”
Inexpensive moist heat reprocessing of N95 respirators inactivates SARS-CoV-2 without harming the structural integrity or function of the mask, even after 10 disinfection cycles, according to data in CMAJ.
July 29, 2020
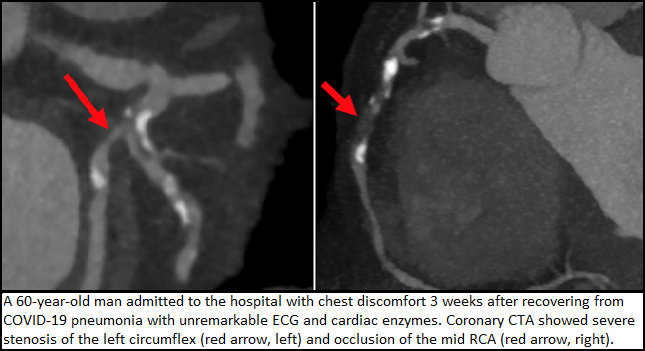 The COVID-19 pandemic has upended the field of cardiac CT imaging and will lead to lasting changes in education, efficiency, and collaboration, experts predicted at the 2020 Society of Cardiovascular Computed Tomography (SCCT) virtual meeting. TCTMD’s Yael Maxwell has the story.
The COVID-19 pandemic has upended the field of cardiac CT imaging and will lead to lasting changes in education, efficiency, and collaboration, experts predicted at the 2020 Society of Cardiovascular Computed Tomography (SCCT) virtual meeting. TCTMD’s Yael Maxwell has the story.
The number of US states considered in the “red zone” for COVID-19 activity has increased to 21, according to the New York Times, which acquired a report sent to state officials by the White House’s coronavirus task force. The report recommends increased restrictions in these states. Only one state, Vermont, is in the “green zone,” with fewer than 10 cases a week per 100,000 people.
An experimental COVID-19 vaccine induced robust immune responses and controlled SARS-CoV-2 in rhesus macaques exposed to the virus, according to results published in the New England Journal of Medicine. It’s the same vaccine candidate, co-developed by Moderna and US government scientists, that was shown to generate an immune response in healthy adults in a phase I trial.
 Whole-genome sequencing and a network/phylogeny analysis of SARS-CoV-2 obtained from pharyngeal specimens indicates that the outbreak on the Diamond Princess cruise ship in early February was caused by single viral introduction, a study in PNAS shows. Of the 3,711 people on board, 697 had developed COVID-19 and seven had died as of March 8.
Whole-genome sequencing and a network/phylogeny analysis of SARS-CoV-2 obtained from pharyngeal specimens indicates that the outbreak on the Diamond Princess cruise ship in early February was caused by single viral introduction, a study in PNAS shows. Of the 3,711 people on board, 697 had developed COVID-19 and seven had died as of March 8.
The next installment of the American College of Cardiology’s free Summer COVID-19 Education Series, will provide an overview of COVID-19 testing for cardiovascular specialists. The session will take place from 12 to 1 pm ET on Thursday, July 30.
Within US metropolitan areas, COVID-19 hits harder in poorer counties and those with more racial/ethnic diversity, but the greater impact in people from minority groups is not fully explained by differences in income, according to a study in JAMA Network Open.
 Also in JAMA Network Open, researchers question how the US Centers for Disease Control and Prevention (CDC) is reporting those racial/ethnic disparities, calling it misleading. “Use of the CDC’s weighted population distributions to evaluate racial/ethnic inequities in COVID-19 mortality underestimates the excess burden of COVID-19 among Black and Latinx individuals compared with analyses conducted using the total population (unweighted) in the US Census data,” they say.
Also in JAMA Network Open, researchers question how the US Centers for Disease Control and Prevention (CDC) is reporting those racial/ethnic disparities, calling it misleading. “Use of the CDC’s weighted population distributions to evaluate racial/ethnic inequities in COVID-19 mortality underestimates the excess burden of COVID-19 among Black and Latinx individuals compared with analyses conducted using the total population (unweighted) in the US Census data,” they say.
July 28, 2020
Tom Frieden, MD, former director of the US Centers for Disease Control and Prevention (CDC) alleges that “most” US states are not reporting vital data needed to properly track the pandemic. According to the BMJ, a report by Resolve to Save Lives, which is led by Frieden, analyzed COVID-19 “dashboards” for all 50 states and the District of Columbia and concluded: “Indicators critical to understanding the pandemic’s course were often missing. . . . Not a single state currently reports the average turnaround time of a polymerase chain reaction test, as press reports abound of tests in many regions taking a week or more to come back, a delay that renders testing nearly useless in controlling the disease’s spread. The test positivity rate goes unreported by 25% of states.”
 Meanwhile Spain and France are reporting new spikes in infection rates, while Belgian authorities are warning that the country may need to go back to “complete lockdown,” the Guardian reports.
Meanwhile Spain and France are reporting new spikes in infection rates, while Belgian authorities are warning that the country may need to go back to “complete lockdown,” the Guardian reports.
The public needs to be protected from research that involves them without consent or lacks critical oversight, researchers argue in the Annals of Internal Medicine. A key part of this is differentiating between activities termed “surveillance” that in fact meet the bar for research, they warn.
Also in Annals, David Sears, MD, and colleagues explore the factors that have made prisons and jails the second-largest source of COVID-19 outbreaks in the United States. “The patchwork of policy and practice that is failing to meet the urgent occupational health crisis that COVID-19 presents in correctional systems should be of particular concern to correctional officers because their unique duties, coupled with the severe overcrowding of US prisons, place them at a level of risk unmatched by an appropriate policy response to protect them,” they say.
Krishna Pundi, MD, and colleagues, writing in JAMA Internal Medicine, examined the quality of evidence being reported in the medical literature in the early months of the COVID-19 pandemic and didn’t like what they saw. “Although a few large multicenter trials may generate high-quality evidence, the large proportion of studies with an expected low level of evidence is concerning,” they conclude. “Rapid dissemination of studies with low-quality evidence studies can influence public opinion, government actions, and clinical practice in potentially harmful ways, especially with a rising tide of COVID-19 study dissemination via preprint or other strategies ahead of peer review.”
 A mathematical modeling study in JAMA Network Open attempts to estimate the room concentration of viral load in droplets from coughing and regular breathing. “Only few people with very high viral load pose an infection risk in poorly ventilated closed environments,” the researchers conclude, advising strict protections for small rooms over prolonged periods.
A mathematical modeling study in JAMA Network Open attempts to estimate the room concentration of viral load in droplets from coughing and regular breathing. “Only few people with very high viral load pose an infection risk in poorly ventilated closed environments,” the researchers conclude, advising strict protections for small rooms over prolonged periods.
The New York Times has profiled Sapan Desai, MD, PhD, “The Doctor Behind the Data” in the two high-profile retractions of an ACE inhibitor/ARB analysis and a hydroxychloroquine study from the New England Journal of Medicine and the Lancet, respectively, both using Surgisphere data. TCTMD covered both.
Polish investigators writing in Catheterization and Cardiovascular Interventions detail the impact of the COVID-19 pandemic and the lockdown on percutaneous coronary interventions over a 2-month period. Like elsewhere, Poland saw a marked decline in procedures, but the investigators say that procedural characteristics and outcomes were similar among patients with versus without confirmed infections.
 According to research in JAMA, more than 2 million Americans stayed home from work for illness in mid-April 2020, the highest figure since at least 1976. Numbers were particularly high for immigrant workers, workers older than 55, and workers with less education. While some of the numbers may be explained by anxiety about infection risks or options for telecommuting, “the findings suggest that the official counts of COVID-19 cases greatly understate the number of people sickened by the virus,” a press release notes.
According to research in JAMA, more than 2 million Americans stayed home from work for illness in mid-April 2020, the highest figure since at least 1976. Numbers were particularly high for immigrant workers, workers older than 55, and workers with less education. While some of the numbers may be explained by anxiety about infection risks or options for telecommuting, “the findings suggest that the official counts of COVID-19 cases greatly understate the number of people sickened by the virus,” a press release notes.
The US Food and Drug Administration (FDA) is warning consumers, yet again, about dangerous hand sanitizers containing methanol that can be toxic when absorbed through the skin, taking the additional step of placing certain products on an import alert. This allows shipments to be detailed without physical examination, the agency notes. They agency is maintaining a list of dangerous sanitizers.
Today's Dispatch was contributed by Shelley Wood.
July 27, 2020
 COVID-19’s hallmark thrombotic risk exists across all hospitalized patients, not just the sickest who require ICU-level care, a study in JAMA suggests. Moreover, TCTMD’s Caitlin Cox reports, these venous and arterial events are accompanied by heightened mortality.
COVID-19’s hallmark thrombotic risk exists across all hospitalized patients, not just the sickest who require ICU-level care, a study in JAMA suggests. Moreover, TCTMD’s Caitlin Cox reports, these venous and arterial events are accompanied by heightened mortality.
Though California remains the state with the highest COVID-19 case count (about 459,000), Florida has jumped over New York into second place (about 424,000), Reuters reports. Globally, Latin America is now the most hard-hit region (accounting for about 27% of all cases) following surges in Brazil, Mexico, Peru, Columbia, and Argentina.
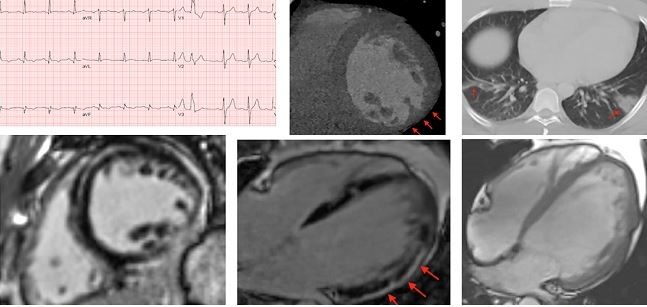
A multispecialty review commissioned by the Cardiovascular Imaging Leadership Council of the American College of Cardiology summarizes the available evidence and offers guidance for multimodal imaging in the setting of cardiac indications and confirmed or possible SARS-CoV-2 infection. “We felt that it might be helpful for clinicians out in the field to get an integrated expert view bringing in all the opinions, not just one subspecialty, and arriving at some consensus about what we think is most effective in this disease,” senior author Marcelo Di Carli, MD, told TCTMD Managing Editor Shelley Wood.
A phase III trial of the investigational COVID-19 vaccine co-developed by Moderna and the US National Institute of Allergy and Infectious Diseases (NIAID) has started. The aim is to enroll about 30,000 adult volunteers. This is the first vaccine efficacy trial initiated as part of the US federal government’s Operation Warp Speed. US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, said, “Having a safe and effective vaccine distributed by the end of 2020 is a stretch goal, but it’s the right goal for the American people.”
Recovery from mild COVID-19 and a return to usual health can be protracted even in younger patients without chronic conditions, a study in Morbidity and Mortality Weekly Report shows. A telephone survey conducted 2 to 3 weeks after a positive SARS-CoV-2 test result showed that 35% of participants had not yet returned to their usual health state, including 20% of those aged 18 to 34.
 Evidence does not support the idea that wearing a face covering leads to people becoming more lax when it comes to other protective measures, researchers argue in the BMJ. “The concept of risk compensation, rather than risk compensation itself, seems the greater threat to public health through delaying potentially effective interventions,” they say.
Evidence does not support the idea that wearing a face covering leads to people becoming more lax when it comes to other protective measures, researchers argue in the BMJ. “The concept of risk compensation, rather than risk compensation itself, seems the greater threat to public health through delaying potentially effective interventions,” they say.
Should SGLT2 inhibition be considered as a COVID-19 treatment? Clinicians should consider “that endothelial/organ damage caused by SARS-CoV-2 results in immune cell activation and cytokine secretion, which can be reduced with the anti-inflammatory properties of SGLT2 inhibitors,” according to correspondence in the Canadian Journal of Cardiology. “Thus, SGLT2 inhibitors may potentially improve outcomes in COVID-19 patients by reducing the organ and/or systemic inflammatory response.”
At the end of March 2020, 40.7% of EMS responders and 34.5% of firefighters from the Fire Department of the City of New York (FDNY) were on medical leave for suspected or confirmed COVID-19, with 1.2% hospitalized and four who had died, a study in JAMA Network Open shows. Medical leave was increased during the pandemic compared with prior years, peaking in the first week of April.
A study in the American Journal of Cardiology provides insights into acute pulmonary embolism in patients hospitalized with COVID-19. Of 101 patients admitted to two hospitals within the Northwell Health system in New York, 23% required ICU admission and 20% required mechanical ventilation. The mortality rate was 20%.
July 24, 2020
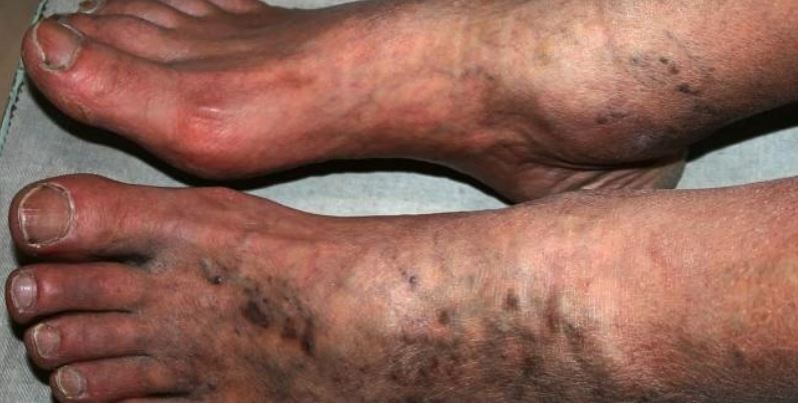
A study in Radiology shows that some patients with COVID-19 develop symptomatic arterial thrombosis in their legs that is difficult to eradicate by usual means and portends worse outcomes, TCTMD’s L.A. McKeown reports. Patients with symptoms of leg ischemia were 25-fold more likely to require amputation or to die if they also had COVID-19. The highest risk was seen in those with a combination of COVID-19, leg ischemia, and pulmonary or systemic symptoms.
The negative hydroxychloroquine data keep coming, with a Brazilian trial showing that the drug, with or without azithromycin, did not improve outcomes in patients with mild-to-moderate COVID-19. According to results published in the New England Journal of Medicine, the treatment increased rates of prolongation of the corrected QT interval and elevation of liver enzyme levels.
The European Medicines Agency (EMA) has started a review of the dexamethasone results from the RECOVERY trial, which indicate that the corticosteroid reduced mortality by about 35% in COVID-19 patients on invasive mechanical ventilation and by about 20% in those receiving oxygen without invasive ventilation. There was no impact in patients not receiving oxygen therapy.
 A video case study in Thorax indicates that a single-layer cloth face covering reduces droplet spread from talking, but that a double-layer covering works better. A double-layer mask was better for reducing droplet spread from coughing and sneezing. A surgical mask was best for all tested scenarios.
A video case study in Thorax indicates that a single-layer cloth face covering reduces droplet spread from talking, but that a double-layer covering works better. A double-layer mask was better for reducing droplet spread from coughing and sneezing. A surgical mask was best for all tested scenarios.
Researchers estimate that the prevalence of any of five underlying conditions that have been associated with an elevated risk of severe COVID-19-related illness—chronic obstructive pulmonary disease, heart disease, diabetes, chronic kidney disease, or obesity—in US adults is 47.2%, with a higher rate in rural counties. The findings, the authors say in Morbidity and Mortality Weekly Report, may help guide decisions about resource allocation and prevention and mitigation strategies.
A study of sex differences in mortality rates and underlying conditions for COVID-19 deaths in England and Wales shows that mortality related to the condition was consistently higher in men than in women across ages. The most common underlying conditions were hypertension, dementia, chronic lung disease, and diabetes, all of which were more frequently seen in COVID-19 deaths. The findings were reported in Mayo Clinic Proceedings.
In an NEJM special report, US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, and colleagues describe the agency’s efforts to rapidly enhance testing technologies for SARS-CoV-2. “Aiming to achieve this rapid evaluation, validation, and scale-up has rarely, if ever, been attempted at this pace,” they write.
 The SARS-CoV-2 virus has been isolated from the mastoid and middle ear, researchers report in JAMA Otolaryngology – Head & Neck Surgery. The study “offers proof of principle of the virus’ ability to access the middle ear and/or mastoid, documents another potential route of SARS-CoV-2 transmission, and addresses the implications for protection of healthcare workers caring for patients with ear disease,” according to an accompanying commentary.
The SARS-CoV-2 virus has been isolated from the mastoid and middle ear, researchers report in JAMA Otolaryngology – Head & Neck Surgery. The study “offers proof of principle of the virus’ ability to access the middle ear and/or mastoid, documents another potential route of SARS-CoV-2 transmission, and addresses the implications for protection of healthcare workers caring for patients with ear disease,” according to an accompanying commentary.
Perinatal transmission of SARS-CoV-2 is not very likely when appropriate hygiene precautions are taken, according to a study in the Lancet Child & Adolescent Health. It suggests “that allowing neonates to room in with their mothers and direct breastfeeding are safe procedures when paired with effective parental education of infant protective strategies,” the authors write.
July 23, 2020
 A recent case report in Circulation suggests nonobstructive chest pain symptoms, presumed to be myocarditis in the setting of COVID-19, may actually be extensive and elusive microthrombi, TCTMD’s Caitlin Cox reports. “This type of injury would not be detectable clinically, as no laboratory test specifically can detect microthrombi,” the researchers say.
A recent case report in Circulation suggests nonobstructive chest pain symptoms, presumed to be myocarditis in the setting of COVID-19, may actually be extensive and elusive microthrombi, TCTMD’s Caitlin Cox reports. “This type of injury would not be detectable clinically, as no laboratory test specifically can detect microthrombi,” the researchers say.
US COVID-19 hospitalizations are nearing the April peak, the New York Times reports. On Wednesday, 59,628 people were hospitalized, just shy of the 59,940 who were being treated in the hospital on April 15, when New York City was the epicenter of the outbreak, according to data from the COVID Tracking Project. NPR’s heat map suggests daily cases are rising in 46 states, led by Louisiana, Mississippi, and Nevada.
There remains a fear of calling 9-1-1 or going to the hospital as the COVID-19 pandemic continues, particularly among Hispanic and Black individuals, according to survey conducted by the Harris Poll on behalf of the American Heart Association (AHA). More than half of Hispanics (55%) and 45% of Black individuals said they would be scared to go to the hospital if they thought they were having an MI or stroke because of a perceived risk of getting infected, compared with 40% of white individuals.
To combat that lingering fear, which they characterize as “an emerging cardiac risk,” Benjamin Wessler, MD, and colleagues say in a JAMA Cardiology viewpoint that “it is essential that hospitals shed the perception of being war zones and redefine themselves as safe zones. We will thereby restore our perceived and actual ability to provide proven, life-saving treatments to patients with other deadly but reversible conditions.”
Experts provide guidance around the use of multimodality imaging in the evaluation of cardiovascular complications in patients with COVID-19 in the Journal of the American College of Cardiology. “Routine history, physical examination, laboratory testing, electrocardiography, and plain X-ray imaging may often suffice for such patients but given overlap between COVID-19 and typical cardiovascular diagnoses such as heart failure and acute myocardial infarction, need frequently arises for advanced imaging techniques to assist in differential diagnosis and management,” they say.
 Solid organ transplants have fallen during the pandemic, and that includes heart transplants, a study in JAMA Cardiology shows. In the COVID-19 era, there was a 75% increase in waitlist inactivations and a 37% reduction in waitlist additions in the United States. The largest decrease in heart transplants was in the Northeast.
Solid organ transplants have fallen during the pandemic, and that includes heart transplants, a study in JAMA Cardiology shows. In the COVID-19 era, there was a 75% increase in waitlist inactivations and a 37% reduction in waitlist additions in the United States. The largest decrease in heart transplants was in the Northeast.
In a JAMA viewpoint, Eva Petkova, MD, and colleagues propose a way to pool data from COVID-19 clinical trials to find safe and effective treatment as quickly as possible. “There is an imperative to find a solution to the mismatch between the location of enrolling sites and the regional incidence of new cases of COVID-19,” they write.
Members of the Advisory Committee on Immunization Practices (ACIP), which provides recommendations on use of vaccines, describe the committee’s role in the pandemic vaccine response in another JAMA viewpoint. “Given the many challenges ahead, maintaining public trust will be crucial before, during, and long after COVID-19 vaccines are deployed for use. Ensuring support for robust public health surveillance systems to monitor vaccine effectiveness and vaccine safety should help to enable a dynamic decision-making process that seeks to improve health, mitigate inequities, and restore stability to society and the economy,” they write.
US Food and Drug Administration (FDA) researchers presented data at the American Association of Clinical Research (AACR) COVID-19 and Cancer meeting showing that cancer patients who also have COVID-19 have a 16-fold increased mortality risk.
 The COVID-19 pandemic has indeed had a detrimental impact on people’s mental health, UK data in the Lancet Psychiatry confirm. Most affected were young people, women, and those living with children.
The COVID-19 pandemic has indeed had a detrimental impact on people’s mental health, UK data in the Lancet Psychiatry confirm. Most affected were young people, women, and those living with children.
The Cleveland Clinic has developed a calculator that estimates a patient’s risk of having a positive COVID-19 test result, taking into account demographic factors, clinical risk factors, zip code, symptoms, comorbidities, and medication use.
A study in JAMA Network Open indicates that social distancing, lower population density, and warmer weather are associated with a lower instantaneous reproduction number (cases generated by each incident case) for SARS-CoV-2.
July 22, 2020
 The COVID-19-linked constellation of symptoms dubbed the multisystem inflammatory syndrome in children (MIS-C) has been increasingly seen around the world, but a smattering of recent reports document what appears to be a very rare but similar presentation in adults, TCTMD’s Shelley Wood reports.
The COVID-19-linked constellation of symptoms dubbed the multisystem inflammatory syndrome in children (MIS-C) has been increasingly seen around the world, but a smattering of recent reports document what appears to be a very rare but similar presentation in adults, TCTMD’s Shelley Wood reports.
For the first time in July, more than 1,000 COVID-19-related deaths—1,120 to be exact—were recorded in a single day in the United States, the New York Times reports. Tuesday’s total was the highest since May 29.
 Observational data from France, published in the European Heart Journal, show that risk factors for pulmonary embolism among patients with COVID-19 diverge from those traditionally observed, but that risk is attenuated by the use of therapeutic doses of anticoagulation at the time of hospitalization, TCTMD’s Yael Maxwell reports.
Observational data from France, published in the European Heart Journal, show that risk factors for pulmonary embolism among patients with COVID-19 diverge from those traditionally observed, but that risk is attenuated by the use of therapeutic doses of anticoagulation at the time of hospitalization, TCTMD’s Yael Maxwell reports.
Correspondence in the New England Journal of Medicine indicates a rapid decay of anti-SARS-CoV-2 antibodies in people with mild cases of COVID-19, which could have implications for “immunity passports,” herd immunity, and vaccine durability. “Our findings raise concern that humoral immunity against SARS-CoV-2 may not be long-lasting in persons with mild illness, who compose the majority of persons with COVID-19,” the authors write.
 On Wednesday, the US Department of Health and Human Services (HHS) and the Department of Defense (DoD) announced an agreement with Pfizer for the production and delivery of 100 million doses of a COVID-19 vaccine for Americans after a safe and effective vaccine is created and cleared for use either through an emergency use authorization or US Food and Drug Administration (FDA) approval. Per the agreement, the US can acquire an additional 500 million doses.
On Wednesday, the US Department of Health and Human Services (HHS) and the Department of Defense (DoD) announced an agreement with Pfizer for the production and delivery of 100 million doses of a COVID-19 vaccine for Americans after a safe and effective vaccine is created and cleared for use either through an emergency use authorization or US Food and Drug Administration (FDA) approval. Per the agreement, the US can acquire an additional 500 million doses.
The presence and extent of coronary artery calcification are associated with worse prognosis hospitalized COVID-19 patients, according to a study in JACC: Cardiovascular Imaging. “The severity of immune response, endothelial dysfunction, and myocardial stress due to COVID-19 could be exacerbated in patients with subclinical coronary atherosclerosis,” the authors conclude.
In June, the European Society of Cardiology’s Cardiovascular Round Table discussed the impact of COVID-19 on cardiovascular research and clinical practice. All of the videos can be found on YouTube.
In the next installment of the American College of Cardiology’s free Summer COVID-19 Education Series, Kim Eagle, MD will moderate a discussion on the current state of research, diagnostic testing, and treatment. The session will take place from 12 to 1 pm ET on Thursday, July 23.
New retrospective data published in the British Journal of Clinical Pharmacology highlight the potential harms of using hydroxychloroquine and azithromycin off-label to treat hospitalized patients with COVID-19. The treatments were not significantly associated with clinical improvement compared with no targeted therapy. Mortality at 28 days and QT prolongation were significantly higher in the treatment group.
 A study in Morbidity and Mortality Weekly Report shows that in Indiana, the estimated prevalence of current of previous SARS-CoV-2 infection in late April was just 2.79%, with a higher rate in Hispanic/Latino individuals. Of people with active infections, 44% did not have any symptoms. Another MMWR report demonstrates that only an estimated 2.5% of the population of two counties in metropolitan Atlanta, GA, had antibodies to SARS-CoV-2 in late April/early May.
A study in Morbidity and Mortality Weekly Report shows that in Indiana, the estimated prevalence of current of previous SARS-CoV-2 infection in late April was just 2.79%, with a higher rate in Hispanic/Latino individuals. Of people with active infections, 44% did not have any symptoms. Another MMWR report demonstrates that only an estimated 2.5% of the population of two counties in metropolitan Atlanta, GA, had antibodies to SARS-CoV-2 in late April/early May.
July 21, 2020
 The wide-ranging cardiac effects during the acute phase of COVID-19 are now well established, but the potential long-term impact of the disease on the heart remains unclear. TCTMD Managing Editor Shelley Wood spoke with researchers looking into that question. “With this disease,” said John P. Greenwood, MBChB, PhD, “we’ve got no idea of what the sort of short- to medium-term outcomes are going to be and certainly no idea what the long-term outcomes are going to be from a heart perspective.”
The wide-ranging cardiac effects during the acute phase of COVID-19 are now well established, but the potential long-term impact of the disease on the heart remains unclear. TCTMD Managing Editor Shelley Wood spoke with researchers looking into that question. “With this disease,” said John P. Greenwood, MBChB, PhD, “we’ve got no idea of what the sort of short- to medium-term outcomes are going to be and certainly no idea what the long-term outcomes are going to be from a heart perspective.”
Within a large health system in New York City, 16% of patients diagnosed with severe SARS-CoV-2 infection had a thrombotic event, including 6.2% with a venous event and 11.1% with an arterial event (patients could have more than one), according to a JAMA research letter. All-cause mortality was twice as high in patients with versus without a thrombotic event (43.2% vs 21.0%).
A temporary hospital set up to treat COVID-19 patients during the height of the pandemic in New York City—built at the USTA Billie Jean King National Tennis Center in Queens—cost more than $52 million but treated only 79 patients, the New York Times reports. The story “illustrates the missteps made at every level of government in the race to create more hospital capacity in New York. It is a cautionary tale for other states now facing surges in cases and for New Yorkers bracing for a possible second wave.”
Data from Italy, published in JAMA Internal Medicine, suggest that the official count of COVID-19 deaths from March and early April substantially understated the actual increase in mortality related directly or indirectly to the pandemic.
 Also in this journal, a cross-sectional seroprevalence study conducted at 10 sites in the United States, based on 16 025 serum samples collected at two commercial labs, concluded that SARS-CoV-2 infections are in the range of 10 times higher than the number of reported cases. “During March to early May 2020, most persons in 10 diverse geographic sites in the US had not been infected with SARS-CoV-2 virus,” the authors conclude. However, “the estimated number of infections ranged from 6 to 24 times the number of reported cases.”
Also in this journal, a cross-sectional seroprevalence study conducted at 10 sites in the United States, based on 16 025 serum samples collected at two commercial labs, concluded that SARS-CoV-2 infections are in the range of 10 times higher than the number of reported cases. “During March to early May 2020, most persons in 10 diverse geographic sites in the US had not been infected with SARS-CoV-2 virus,” the authors conclude. However, “the estimated number of infections ranged from 6 to 24 times the number of reported cases.”
The European Medicines Agency has set up infrastructure for the monitoring of the safety and effectiveness of COVID-19 treatments and vaccines in everyday practice: “This is underpinned by three contracts for observational research that EMA has signed with academic and private partners over recent months, to be ready to effectively monitor vaccines in the real world as soon as they are authorized, and support the safe and effective use of COVID-19 vaccines and medicines,” a statement reads.
German physicians saw an uptick in the frequency of diabetic ketoacidosis and severe ketoacidosis at diabetes diagnosis in children and adolescents during the first 2 months of the pandemic. In a JAMA research letter, they say the “underlying causes may be multifactorial and reflect reduced medical services, fear of approaching the healthcare system, and more complex psychosocial factors.”
Could use of tenecteplase instead of alteplase for stroke thrombolysis have a role in reducing the spread of SARS-CoV-2 in emergency departments? Steven Warach, MD, and Jeffrey Saver, MD, make the case in JAMA Neurology.
 A modeling study in the Lancet Oncology indicates that diagnostic delays due to the pandemic will increase the number of deaths from four cancer types—breast, colorectal, esophageal, and lung—in England over the next 5 years. Another modeling study in the same journal concludes: “Prompt provision of additional capacity to address the backlog of diagnostics will minimize deaths as a result of diagnostic delays that could add to those predicted due to expected presentational delays.”
A modeling study in the Lancet Oncology indicates that diagnostic delays due to the pandemic will increase the number of deaths from four cancer types—breast, colorectal, esophageal, and lung—in England over the next 5 years. Another modeling study in the same journal concludes: “Prompt provision of additional capacity to address the backlog of diagnostics will minimize deaths as a result of diagnostic delays that could add to those predicted due to expected presentational delays.”
In a blog post, US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, describes how genome data can help track community spread of SARS-CoV-2.
July 20, 2020
 A study in the Journal of the American College of Cardiology (JACC) shows that as COVID-19 battered New York earlier this year, the city saw an upswing in out-of-hospital cardiac arrest cases that correlated with a decrease in hospitalizations for acute coronary syndromes, TCTMD’s Caitlin Cox reports. “I think the important message is: even in COVID, emergencies are still emergencies. People need to seek care, because it’s more dangerous not to seek care, despite COVID,” the senior author said.
A study in the Journal of the American College of Cardiology (JACC) shows that as COVID-19 battered New York earlier this year, the city saw an upswing in out-of-hospital cardiac arrest cases that correlated with a decrease in hospitalizations for acute coronary syndromes, TCTMD’s Caitlin Cox reports. “I think the important message is: even in COVID, emergencies are still emergencies. People need to seek care, because it’s more dangerous not to seek care, despite COVID,” the senior author said.
The Johns Hopkins COVID-19 Dashboard lists 14.5 million confirmed COVID-19 cases worldwide, with the top number coming from the United States (nearly 3.8 million). Florida is being hit hard, with CBS News reporting that at least 45 hospitals in the state had no available ICU beds as of Sunday afternoon.
TCTMD Managing Editor Shelley Wood provides additional details on the RECOVERY trial of dexamethasone published last week in the New England Journal of Medicine. Though treatment lowered the risk of mortality in patients receiving respiratory support, it did not impact outcomes in patients who did not require such support.
 The high thrombus burden seen in COVID-19 patients who present with STEMI “may be related to increased platelet activation, possibly endothelial dysfunction, or the direct effects of the virus on the immune system,” the author of a recent JACC paper told TCTMD’s Michael O’Riordan.
The high thrombus burden seen in COVID-19 patients who present with STEMI “may be related to increased platelet activation, possibly endothelial dysfunction, or the direct effects of the virus on the immune system,” the author of a recent JACC paper told TCTMD’s Michael O’Riordan.
Researchers have reported positive phase I/II data on candidate SARS-CoV-2 vaccines in the Lancet. A British phase I/II trial showed that the vaccine, which expresses the spike protein of the novel coronavirus, induced strong antibody and T-cell immune responses in 1,077 healthy adults, with no serious adverse events. And a Chinese phase II trial demonstrated that a recombinant adenovirus type-5-vectored vaccine safely inducted an immune response in more than 500 participants. “The results of both studies augur well for phase III trials, where the vaccines must be tested on much larger populations of participants to assess their efficacy and safety,” according to an accompanying editorial.
In Mayo Clinic Proceedings, investigators provide an update on the safety of using convalescent plasma for the treatment of patients hospitalized with COVID-19, this time in a sample of 20,000 patients. Serious adverse events were infrequent; they included transfusion reactions (< 1%), thromboembolic or thrombotic events (< 1%), and cardiac events (about 3%). The mortality rate at 7 days was 8.6%. “These updated data provide robust evidence that transfusion of convalescent plasma is safe in hospitalized patients with COVID-19, and support the notion that earlier administration of plasma within the clinical course of COVID-19 is more likely to reduce mortality,” the authors say.
More reassurance about the use of ACE inhibitors/ARBs in the setting of COVID-19 has come from a meta-analysis of 14 studies (excluding the disputed analysis from Mehra et al) published in the European Heart Journal: Cardiovascular Pharmacotherapy. Use of the drugs was not associated with an increased risk of all-cause mortality or severe disease.
 SARS-Cov-2 RNA has been found in a healthy blood donor 40 days after resolution of their COVID-19 symptoms, according to a case report in the Annals of Internal Medicine. This “is concerning in light of current guidelines, which do not recommend SARS-CoV-2 screening in the general allogeneic donor population,” the authors write.
SARS-Cov-2 RNA has been found in a healthy blood donor 40 days after resolution of their COVID-19 symptoms, according to a case report in the Annals of Internal Medicine. This “is concerning in light of current guidelines, which do not recommend SARS-CoV-2 screening in the general allogeneic donor population,” the authors write.
For the first time, the US Food and Drug Administration (FDA) has given the go-ahead to use sample pooling for COVID-19 diagnostic testing, issuing an emergency use authorization to Quest Diagnostics for its Quest SARS-CoV-2 rRT-PCR test. The test can be used with pooled samples containing up to four individual swab specimens collected under observation.
Rates of a return of spontaneous circulation with prehospital CPR declined in April 2020 compared with a similar time period in the preceding 3 years, to 42.95% from about 47%, according to data in Resuscitation. The findings “likely indicate that either CPR quality has decreased or patients are somehow responding less favorably to the current conventions of resuscitation,” the authors say.

In an Arts and Medicine piece in JAMA, researchers describe how Amabié, “a legendary mermaid-like creature who is said to emerge from the sea to prophesize good harvests and epidemics,” has emerged as a symbol of the COVID-19 pandemic in Japan. Twitter brings the legend to life.
July 17, 2020
 COVID-19 patients whose body mass index places them just over the threshold for obesity are at higher risk of developing respiratory failure and being admitted to an intensive care unit compared with normal-weight individuals with the disease, observational data from Italy confirm. People with obesity “should be considered a population at risk,” the lead author told TCTMD’s Caitlin Cox, adding, “They should take extra care regarding their social behavior, distancing. . . . They should use masks. They should avoid risky situations, such as gatherings.”
COVID-19 patients whose body mass index places them just over the threshold for obesity are at higher risk of developing respiratory failure and being admitted to an intensive care unit compared with normal-weight individuals with the disease, observational data from Italy confirm. People with obesity “should be considered a population at risk,” the lead author told TCTMD’s Caitlin Cox, adding, “They should take extra care regarding their social behavior, distancing. . . . They should use masks. They should avoid risky situations, such as gatherings.”
Results of the comparison of dexamethasone with usual care in hospitalized patients with COVID-19 in the RECOVERY trial, previously released in a press release, have been published in the New England Journal of Medicine. Overall, the 28-day mortality rate was lower in dexamethasone-treated patients (22.9% vs 25.7%; age-adjusted rate ratio 0.83; 95% CI 0.75-0.93). The benefits were confined to those receiving either invasive mechanical ventilation or oxygen support without invasive mechanical ventilation.
Hydroxychloroquine did not improve outcomes among nonhospitalized adults with early COVID-19 in a randomized trial, according to results published in the Annals of Internal Medicine. Change in symptom severity over 14 days did not differ between the hydroxychloroquine and placebo groups.

Acute decompensated heart failure-related emergency department visits and admissions fell by roughly 40% during the pandemic compared with the year prior in a hospital in Toronto, Canada, researchers report in the Canadian Journal of Cardiology. The finding “raises the timely question of how patients with heart failure are managing beyond the acute care setting and reinforces the need for public education on the availability and safety of emergency services throughout the COVID-19 pandemic,” they say.
New data from the Centers for Disease Control and Prevention (CDC) confirm prior studies indicating that most of the earliest COVID-19 cases identified in New York City could be traced to Europe, other US states, and local introductions from within New York.
Earlier this week, the US Department of Health and Human Services (HHS) told hospitals that they should report COVID-19 data directly to the agency and not to HHS and the Centers for Disease Control and Prevention (CDC), as had been done before, in order to help better allocate supplies and drugs. A STAT story tackles the implications: “Nearly everyone had questions about how, exactly, it would all work. And days later, the nation’s top public health experts are still scrambling to figure out how seriously this new policy change will impact the COVID-19 response in the US.”
 The Center for Public Integrity, a nonprofit newsroom in Washington, DC, reports that a document prepared for the White House coronavirus task force but not released publicly states that 18 US states are in the “red zone” for COVID-19 cases (more than 100 new cases per 100,000 population) and 11 are in the “red zone” for test positivity (more than 10% of tests are positive). The document recommends that Georgia, which falls into both categories, should mandate face coverings outside the home. On Wednesday, however, Georgia Governor Brian Kemp signed an executive order banning municipalities from enacting their own face-covering mandates, the Washington Post reports.
The Center for Public Integrity, a nonprofit newsroom in Washington, DC, reports that a document prepared for the White House coronavirus task force but not released publicly states that 18 US states are in the “red zone” for COVID-19 cases (more than 100 new cases per 100,000 population) and 11 are in the “red zone” for test positivity (more than 10% of tests are positive). The document recommends that Georgia, which falls into both categories, should mandate face coverings outside the home. On Wednesday, however, Georgia Governor Brian Kemp signed an executive order banning municipalities from enacting their own face-covering mandates, the Washington Post reports.
Intelligence agencies in the United States, the United Kingdom, and Canada say that Russian hackers are trying to steal data related to the development of a COVID-19 vaccine, NPR reports.
Contrast echocardiography is feasible in patients receiving veno-venous extracorporeal membrane oxygenation for severe acute respiratory failure (SARF) related to COVID-19, researchers report in a letter in the Journal of the American Society of Echocardiography. “Appropriate protocols should be instituted at centers offering VV-ECMO, ensuring safe management of the circuit by the perfusion team,” they write. “Enhanced echocardiography may therefore be an appropriate bedside technique during the current viral surge in critical VV-ECMO supported SARF, helping to address diagnostic uncertainty in cases with challenging echocardiography visualization.”
A study in Morbidity and Mortality Weekly Report confirms that fever, cough, and shortness of breath are common symptoms among US COVID-19 patients. GI symptoms, chills, myalgia, headache, and fatigue were also frequently reported.
 Speedy testing is critical to the success of contact-tracing strategies meant to slow the spread of SARS-CoV-2, according to a study in the Lancet Public Health. “In our model, minimizing testing delay had the largest impact on reducing onward transmissions,” the researchers say.
Speedy testing is critical to the success of contact-tracing strategies meant to slow the spread of SARS-CoV-2, according to a study in the Lancet Public Health. “In our model, minimizing testing delay had the largest impact on reducing onward transmissions,” the researchers say.
July 16, 2020
STEMI patients with versus without COVID-19 have higher levels of troponin T, D-dimer, and C-reactive protein, a lower lymphocyte count, and higher rates of multivessel thrombosis and stent thrombosis, according to a study in the Journal of the American College of Cardiology. In these patients, “there is a strong signal towards higher thrombus burden and poorer outcomes,” the authors say.
 Last month, RECOVERY investigators announced that they would no longer enroll patients into the hydroxychloroquine arm of the trial after a look at the data indicated no impact on risk of 28-day mortality or duration of hospital stay. They’ve now published their preliminary findings on a preprint server, showing that hydroxychloroquine-treated patients were less likely to be discharged from the hospital alive within 28 days and—among those not on mechanical ventilation at baseline—were more likely to progress to invasive mechanical ventilation or death compared with patients receiving usual care.
Last month, RECOVERY investigators announced that they would no longer enroll patients into the hydroxychloroquine arm of the trial after a look at the data indicated no impact on risk of 28-day mortality or duration of hospital stay. They’ve now published their preliminary findings on a preprint server, showing that hydroxychloroquine-treated patients were less likely to be discharged from the hospital alive within 28 days and—among those not on mechanical ventilation at baseline—were more likely to progress to invasive mechanical ventilation or death compared with patients receiving usual care.
Two studies in JAMA Internal Medicine, one from the United States and one from Italy, explore risk factors associated with mortality in critically ill patients with COVID-19. Factors included older age, male sex, higher body mass index, CAD, active cancer, hypoxemia, liver dysfunction, kidney dysfunction, history of chronic obstructive pulmonary disease, hypercholesterolemia, and type 2 diabetes.
The July 15, 2020, issue of JACC: Case Reports contains COVID-19-related papers involving sinus node dysfunction in a young patient, a transient Brugada-like ECG pattern in a 61-year-old man, a finding of high-degree AV block without evidence of overt myocarditis, electrical storm, cardiac dysfunction and shock in pediatric patients, and more.
 New data in the BMJ confirm the importance of physical distancing measures—such as closing schools, workplaces, and public transportation, as well as restricting mass gatherings and public events—in reducing the number of COVID-19 cases. Earlier implementation of lockdowns was associated with a greater reduction in cases. “These findings might support policy decisions as countries prepare to impose or lift physical distancing measures in current or future epidemic waves,” the researchers say.
New data in the BMJ confirm the importance of physical distancing measures—such as closing schools, workplaces, and public transportation, as well as restricting mass gatherings and public events—in reducing the number of COVID-19 cases. Earlier implementation of lockdowns was associated with a greater reduction in cases. “These findings might support policy decisions as countries prepare to impose or lift physical distancing measures in current or future epidemic waves,” the researchers say.
For STAT, Juliet Isselbacher delves into how low-dose radiation therapy is being studied as a potential treatment for COVID-19 based on older data showing that the approach was successful in treating pneumonia. There are at least a dozen trials evaluating the approach around the world, she reports.
The National Academies of Sciences, Engineering, and Medicine released a report stating that school districts should prioritize reopening schools full time, especially for children in kindergarten through fifth grade and for those with special needs. “Opening schools will benefit families beyond providing education, including by supplying child care, school services, meals, and other family supports. Without in-person instruction, schools risk children falling behind academically and exacerbating educational inequities,” a press release states.
In a JAMA Psychiatry viewpoint, Alison Hermann, MD, and colleagues discuss the challenges of maternal mental healthcare in obstetric and psychiatric settings during the pandemic and suggest ways to mitigate health risks. “With appropriate coordination as well as robust institutional and collegial investment, we can build resiliency and meaningfully support our patients and each other as health care clinicians in the midst of this crisis,” they write.
 Researchers describe variants of enanthem (oral cavity lesions) in a series of COVID-19 patients with skin rash in JAMA Dermatology. “Despite the increasing reports of skin rashes in patients with COVID-19, establishing an etiological diagnosis is challenging,” they write. “However, the presence of enanthem is a strong clue that suggests a viral etiology rather than a drug reaction, especially when a petechial pattern is observed.”
Researchers describe variants of enanthem (oral cavity lesions) in a series of COVID-19 patients with skin rash in JAMA Dermatology. “Despite the increasing reports of skin rashes in patients with COVID-19, establishing an etiological diagnosis is challenging,” they write. “However, the presence of enanthem is a strong clue that suggests a viral etiology rather than a drug reaction, especially when a petechial pattern is observed.”
The US Food and Drug Administration (FDA) continues to warn consumers about the risk of methanol contamination in certain hand sanitizers as recall notices keep rolling in. Here’s the list of affected products.
July 15, 2020
 Acute ischemic strokes that occur in conjunction with COVID-19 are more severe and carry greater disability than those in patients who don’t have the viral disease, data from the Global COVID-19 Stroke Registry show. “One way I think of it is that stroke is a bad disease, COVID is a bad disease—and you put them together and you’re going to do worse,” American Heart Association (AHA) President Mitchell Elkind, MD, told TCTMD’s Caitlin Cox.
Acute ischemic strokes that occur in conjunction with COVID-19 are more severe and carry greater disability than those in patients who don’t have the viral disease, data from the Global COVID-19 Stroke Registry show. “One way I think of it is that stroke is a bad disease, COVID is a bad disease—and you put them together and you’re going to do worse,” American Heart Association (AHA) President Mitchell Elkind, MD, told TCTMD’s Caitlin Cox.
 And speaking of AHA, this year’s Scientific Sessions, slated to be held in Dallas, TX, in November, will be held virtually instead due to the continuing threat from COVID-19, the organization announced Wednesday. The online event will run from November 13 to 17.
And speaking of AHA, this year’s Scientific Sessions, slated to be held in Dallas, TX, in November, will be held virtually instead due to the continuing threat from COVID-19, the organization announced Wednesday. The online event will run from November 13 to 17.
A universal masking policy at the Mass General Brigham healthcare system was associated with a significantly lower rate of SARS-CoV-2 positivity among healthcare workers, according to a research letter in JAMA.
An editorial accompanying that research letter by physicians from the US Centers for Disease Control and Prevention (CDC), including Director Robert Redfield, MD, points to two new papers in Morbidity and Mortality Weekly Report that address use of face masks: one showing an increase in use of masks by Americans after recommendations from the federal government and the other indicating that universal wearing of masks helped prevent transmission of SARS-CoV-2 from two symptomatic hair stylists to 139 clients. “At this critical juncture when COVID-19 is resurging, broad adoption of cloth face coverings is a civic duty, a small sacrifice reliant on a highly effective low-tech solution that can help turn the tide favorably in national and global efforts against COVID-19,” the editorialists write.
…broad adoption of cloth face coverings is a civic duty, a small sacrifice reliant on a highly effective low-tech solution that can help turn the tide favorably in national and global efforts against COVID-19. Robert Redfield
The greater impact of the pandemic on people from racial/ethnic minority groups appears to be related, at least in part, to the increased risk of exposure to SARS-CoV-2 at work and home, an analysis in Health Affairs indicates. Black individuals at high risk for severe illness were 1.6 times more likely than their white counterparts to live in households that included health-sector workers. And Hispanic and Black adults were more likely to live in households in which at least one worker was unable to work from home.
A case report in Nature Communications details the first instance of SARS-CoV-2 being transmitted by a pregnant mother to her fetus, “confirmed by comprehensive virological and pathological investigations.” When the baby boy was 3 days old, he presented with irritability, poor feeding, axial hypertonia, and opisthotonos. Both the mother and baby have since recovered.
The next installment of the American College of Cardiology’s free Summer COVID-19 Education Series will tackle lessons learned about COVID-19 based on global experience, including discussions about extrapulmonary effects, conservation of personal protective equipment, the search for treatments, and what the pandemic looks like in Africa. The session will take place from 12 to 1 pm ET on Thursday, July 16.
The US Food and Drug Administration (FDA) added dexamethasone, which showed benefits in certain COVID-19 patients in the RECOVERY trial, to its lists of drugs for temporary compounding by outsourcing facilities and pharmacy compounders during the public health emergency. The move is meant to address shortages and access concerns, the agency said.
 A SARS-CoV-2 vaccine candidate from Moderna has been shown to generate an immune response in healthy adults in a phase I trial supported by the US National Institute of Allergy and Infectious Diseases (NIAID), a preliminary report in the New England Journal of Medicine shows. There were no serious adverse events, but more than half of participants reported fatigue, headache, chills, myalgia, or injection-site pain. A phase II trial started in May and there are plans for a phase III trial to start this month.
A SARS-CoV-2 vaccine candidate from Moderna has been shown to generate an immune response in healthy adults in a phase I trial supported by the US National Institute of Allergy and Infectious Diseases (NIAID), a preliminary report in the New England Journal of Medicine shows. There were no serious adverse events, but more than half of participants reported fatigue, headache, chills, myalgia, or injection-site pain. A phase II trial started in May and there are plans for a phase III trial to start this month.
In Clinical Infectious Diseases, researchers discuss three potential uses of human challenge trials, which expose volunteers to an infectious dose of a pathogen, to accelerate SARS-CoV-2 vaccine development—to evaluate efficacy, to determine correlates of protection, and to improve our understanding of pathogenesis and the human immune response. “Despite limitations, human challenge trials could accelerate a SARS-CoV-2 vaccine by providing signals of vaccine efficacy in as little as 2 months or by identifying surrogates of protection,” they write. “Trial preparations would take many months and hence should be started immediately.”
 Symptom-based testing alone is not adequate to identify positive residents of long-term care facilities, researchers say in a research letter in JAMA Internal Medicine. “Additional testing resources are urgently needed to identify the true burden of COVID-19 and curb transmission in long-term care settings,” they conclude.
Symptom-based testing alone is not adequate to identify positive residents of long-term care facilities, researchers say in a research letter in JAMA Internal Medicine. “Additional testing resources are urgently needed to identify the true burden of COVID-19 and curb transmission in long-term care settings,” they conclude.
July 14, 2020
 COVID-19 has wide-ranging effects on the body, affecting the heart, kidneys, brain, endocrine system, and more, according to a study in Nature Medicine. “As we were going through this, seeing the patients in front of us, it really was quite astounding to see the significant ramifications this virus had on these other systems,” one of the report’s lead authors told TCTMD’s Michael O’Riordan.
COVID-19 has wide-ranging effects on the body, affecting the heart, kidneys, brain, endocrine system, and more, according to a study in Nature Medicine. “As we were going through this, seeing the patients in front of us, it really was quite astounding to see the significant ramifications this virus had on these other systems,” one of the report’s lead authors told TCTMD’s Michael O’Riordan.
A case report in the Lancet describes a man who presented with a Kawasaki-like multisystem inflammatory syndrome in the setting of SARS-CoV-2 infection, which is similar to the condition that has been described in children during the pandemic (dubbed MIS-C). “Although we caution readers from making broad conclusions from this single case, we report this presentation to heighten awareness of the possibility of [this] condition in adults,” the researchers write.
Among patients diagnosed with COVID-19, use of ACE inhibitors and ARBs is not associated with a greater risk of hospital admission or with all-cause mortality, ICU stay, need for ventilation, or inotrope use, according to a retrospective study in the American Journal of Cardiology.
 Writing in STAT, Helen Branswell discusses how to fix the US response to COVID-19, which she describes as “a raging dumpster fire.” She writes, “One thing is clear, according to public health experts: Widespread returns to lockdown must be a last resort—and may not be doable.”
Writing in STAT, Helen Branswell discusses how to fix the US response to COVID-19, which she describes as “a raging dumpster fire.” She writes, “One thing is clear, according to public health experts: Widespread returns to lockdown must be a last resort—and may not be doable.”
The COVID-19 pandemic might lead to increasing deaths due to HIV, tuberculosis, and malaria in low- and middle-income countries, stemming from disruptions in typical management activities, according to a modeling study in the Lancet Global Health. “These disruptions could lead to a loss of life-years over 5 years that is of the same order of magnitude as the direct impact from COVID-19 in places with a high burden of malaria and large HIV and tuberculosis epidemics,” the authors say.
In a JAMA viewpoint, researchers detail theoretical considerations and available evidence around the airborne transmission of SARS-CoV-2. The understanding of how the virus is transmitted remains limited, they say. “It is impossible to conclude that aerosol-based transmission never occurs and it is perfectly understandable that many prefer to err on the side of caution, particularly in healthcare settings when caring for patients with suspected or confirmed COVID-19,” they write. “However, the balance of currently available evidence suggests that long-range aerosol-based transmission is not the dominant mode of SARS-CoV-2 transmission.”
A survey of more than 5,800 small businesses conducted between March 28 and April 4, 2020, showed that mass layoffs and closures had already occurred and many were already financially fragile, with little available cash with which to weather the crisis. “Small businesses’ responses to our survey suggest that many are likely to fail absent financial assistance,” the authors write in PNAS.
 In a JAMA Internal Medicine viewpoint, Sarah Sy, MD, and Medha Munshi, MD, discuss the challenges of caring for older adults with diabetes during the pandemic and offer practical recommendations. One proactive step they recommend is “to identify ‘high-risk’ patients (eg, type 1 diabetes, recurrent hypoglycemia), prioritize patient goals, provide repeated education, and reassess the diabetes treatment plan to lower disease and treatment burden.”
In a JAMA Internal Medicine viewpoint, Sarah Sy, MD, and Medha Munshi, MD, discuss the challenges of caring for older adults with diabetes during the pandemic and offer practical recommendations. One proactive step they recommend is “to identify ‘high-risk’ patients (eg, type 1 diabetes, recurrent hypoglycemia), prioritize patient goals, provide repeated education, and reassess the diabetes treatment plan to lower disease and treatment burden.”
The Academy of Medical Sciences has warned that the United Kingdom needs to prepare now for a winter peak in COVID-19 cases to prevent a doubling in the number of hospital deaths compared with the first wave, according to a news story in the BMJ: “The academy called for ‘intense preparation’ throughout the rest of July and August to reduce the risk of the NHS being overwhelmed and to save lives this winter.”
Amnesty International has released a report documenting the experiences of healthcare workers around the world during the COVID-19 pandemic; its analysis shows that more than 3,000 are known to have died from the disease. “States must ensure adequate compensation for all health and essential workers who have contracted COVID-19 as a result of work-related activities,” a press release states. “They must also investigate cases where workers have faced reprisals for raising health and safety concerns, and provide effective remedy to those who have been unjustly treated, including by reinstating workers who have lost their jobs for speaking out.”
Having a multitude of randomized trials exploring similar research questions during the pandemic increases the likelihood of positive findings through chance alone and may compromise enrollment of sufficient numbers of patients for any given study, researchers say in JAMA Network Open. “Together, these factors endanger the capacity to rapidly produce meaningful evidence that is vital during this critical time,” the authors say. “Avoiding these pitfalls requires coordination of efforts.”
July 13, 2020

Critically ill COVID-19 patients treated with the intravenous IL-6 blocker tocilizumab were 45% less likely to die and more likely to be off a ventilator and discharged from hospital within a month compared with patients not given the drug, a single-center study shows. That’s despite a doubling of the risk of super-infections among patients taking the agent, authors write in Clinical Infectious Diseases. “Tocilizumab, originally designed for rheumatoid arthritis, has already been used to calm [cytokine] storms in patients receiving advanced immunotherapy treatment for cancer,” a press release notes.
Newspapers around the world took note of President Donald Trump wearing a face mask for the first time—in a visit to wounded service members at Walter Reed National Military Medical Center. That comes as coronavirus cases in the United States increased in 39 states this weekend, with total cases topping 3.3 million and deaths inching close to 135,000, the New York Times reports. Also in the Times, health officials in Hong Kong have announced that a rise in local transmissions means they will close gyms, shutter cinemas, and ban public gatherings of more than four people. According to the Guardian, there have been 11 new deaths in England, with no new deaths in Scotland or Wales.
 Smoking and e-cigarette use are key predictors of disease severity in young people infected with SARS-CoV-2 and can lead to severe disease in one in three young adults, investigators report in the Journal of Adolescent Health. Using a nationally representative ample of 8,400 adults aged 18-25, Sally Adams, PhD, RN, et al found that “medical vulnerability” to severe COVID-19, based on the presence of other risks factors such as asthma, diabetes, and obesity, was just 16.1% for nonsmokers but rose to 31.5% when smokers were including in the sample.
Smoking and e-cigarette use are key predictors of disease severity in young people infected with SARS-CoV-2 and can lead to severe disease in one in three young adults, investigators report in the Journal of Adolescent Health. Using a nationally representative ample of 8,400 adults aged 18-25, Sally Adams, PhD, RN, et al found that “medical vulnerability” to severe COVID-19, based on the presence of other risks factors such as asthma, diabetes, and obesity, was just 16.1% for nonsmokers but rose to 31.5% when smokers were including in the sample.
A new review in JAMA summarizes the evidence to date on the pathophysiology, transmission, diagnosis, and management of COVID-19. “As of July 1, 2020, more than 10 million people worldwide had been infected with SARS-CoV-2,” W. Joost Wiersinga, MD, PhD, and colleagues write. “Many aspects of transmission, infection, and treatment remain unclear.”
 “While many low and middle income (LMI) countries are currently lifting the lockdowns due to economic reasons, it is crucial for the policy makers to recognize that preserving health is equally important for reviving the economy” in these nations, an international team of researchers argue in the European Journal of Epidemiology. The sustained mitigation measures adopted by higher-income countries (mask wearing, physical distancing, and the isolation of positive cases after testing) are less feasible in LMI nations, whereas zonal lockdowns of outbreak clusters or “rolling lockdowns” involving strict isolation for a number of weeks followed by a period of relaxation may slow transmission and ease the burden on limited healthcare systems.
“While many low and middle income (LMI) countries are currently lifting the lockdowns due to economic reasons, it is crucial for the policy makers to recognize that preserving health is equally important for reviving the economy” in these nations, an international team of researchers argue in the European Journal of Epidemiology. The sustained mitigation measures adopted by higher-income countries (mask wearing, physical distancing, and the isolation of positive cases after testing) are less feasible in LMI nations, whereas zonal lockdowns of outbreak clusters or “rolling lockdowns” involving strict isolation for a number of weeks followed by a period of relaxation may slow transmission and ease the burden on limited healthcare systems.
The number of stillbirths increased significantly between February 1 and June 14, 2020, at St George’s University Hospital in London as compared with a historical period. However, “none of the pregnant women who experienced stillbirth had symptoms suggestive of COVID-19, nor did the postmortem or placental examinations suggest SARS-CoV-2 infection,” authors of a research letter write in JAMA. Asymptomatic infections cannot be ruled out, but changes to obstetric services due to staff shortages or cancelled surveillance appointments, as well as hospital avoidance, likely played a role.
 Fear of touching others during the current pandemic could result in a devastating decline in bystander CPR, an article in Circulation warns. Addressing concerns and training the public in “best practices to maintain one’s personal safety” should be the focus moving forward.
Fear of touching others during the current pandemic could result in a devastating decline in bystander CPR, an article in Circulation warns. Addressing concerns and training the public in “best practices to maintain one’s personal safety” should be the focus moving forward.
Contributed today by Shelley Wood and L.A. McKeown.
July 10, 2020
TCTMD’s Todd Neale reports on a review paper that offers a frame for how to use troponin testing in patients with COVID-19. Elevated levels suggestive of myocardial injury have been frequently reported in coronavirus patients and can help clinicians to “identify those people who were really getting into trouble,” a co-author said.
The World Health Organization (WHO) will conduct an independent review of global response to the COVID-19 pandemic. The effort will be led by Liberian President Ellen Johnson Sirleaf, winner of the Nobel Peace Prize, and Helen Clark, former Prime Minister of New Zealand. An interim report is expected by November, with a “substantive” report to the WHO’s governing body in May 2021, STAT reports.

Among Italian patients who have recovered from COVID-19, 87.4% report having at least one persistent symptom at 60 days. Writing in JAMA, the investigators say the most common lingering symptoms are fatigue (53.1%), dyspnea (43.4%), joint pain, (27.3%) and chest pain (21.7%).
In a cross-sectional analysis of COVID-19-related papers published over an 80-day period, the number of opinion articles was more than three times greater than the number of original investigations. According to the report published in the Journal of General Internal Medicine, “medical journals might want to re-evaluate the usefulness of COVID-19-related opinion pieces being considered for publication.”
A report in the American Journal of Managed Care confirms that some patients may be deferring necessary medical care for urgent conditions. Comparing daily hospital admission rates for March and April 2020 with those for March and April 2019, a cross-sectional study found a 33.7% decrease in admission rates for all conditions combined. The authors suggest that there is an urgent need for public awareness campaigns “to reassure the public about the safety of presenting for care.”
 School superintendents across the United States are facing many challenges as they balance safe reopening of schools with protecting the health of their students and staff in the midst of the pandemic. An article in JAMA outlines how superintendents are working to provide Wi-Fi to students whose families can’t afford it, space seating and group activities according to Centers for Disease Control and Prevention (CDC) guidelines, avoid in-person meetings between teachers and staff, hold as many classes outdoors as possible, and debate widespread testing and protocols to monitor for COVID-19 symptoms.
School superintendents across the United States are facing many challenges as they balance safe reopening of schools with protecting the health of their students and staff in the midst of the pandemic. An article in JAMA outlines how superintendents are working to provide Wi-Fi to students whose families can’t afford it, space seating and group activities according to Centers for Disease Control and Prevention (CDC) guidelines, avoid in-person meetings between teachers and staff, hold as many classes outdoors as possible, and debate widespread testing and protocols to monitor for COVID-19 symptoms.
In BMJ Case Reports, researchers describe a 49-year-old man with no significant medical history who developed Guillain-Barré syndrome associated with COVID-19 infection. After a 3-week history of shortness of breath, headache and cough, and two courses of antibiotics, the man presented with muscle weakness and mobility issues that worsened until he was unable to walk. He was treated with IV immunoglobulin and slowly regained his ability to walk unassisted. The researchers say Guillain-Barré “should be considered as a potential rare but serious complication weeks after initial COVID-19 infection.”
A survey in JAMA Ophthalmology of 84 ophthalmologists and 42 ophthalmic nurses who were working in Wuhan, China, during the COVID-19 outbreak found that they suffered from more anxiety and depression compared with colleagues working in an area that was not as hard-hit by the virus. The Wuhan workers also had eye-related symptoms such as dryness, foreign-body sensation, redness, and burning. The cause of the symptoms is unclear, but may have been the result of having to wear eye protection for long periods of time or getting poor-quality sleep. “It also remains unknown if the reported symptoms of anxiety or depression may have led to greater perception of dry eye symptoms or a greater likelihood to rate their symptoms more severely,” the researchers write.
A retrospective study of ACS patients presenting in March and April 2020 found that they had a significant increase stress cardiomyopathy compared with patients presenting with ACS at multiple timepoints prior to the COVID-19 pandemic. Writing in JAMA Network Open, the authors say all patients with stress cardiomyopathy tested negative for the virus, which suggests “an indirect, psychological, social, and economic pandemic-related stress mechanism behind the disease process.”
 New data published in Morbidity and Mortality Weekly report show only a minor impact of COVID-19 on health-related workplace absenteeism. However, in April 2020, absenteeism was significantly higher than expected among certain essential worker categories, specifically those in healthcare support, personal care and service occupations, and production occupations.
New data published in Morbidity and Mortality Weekly report show only a minor impact of COVID-19 on health-related workplace absenteeism. However, in April 2020, absenteeism was significantly higher than expected among certain essential worker categories, specifically those in healthcare support, personal care and service occupations, and production occupations.
July 9, 2020
 TCTMD’s Caitlin Cox reports on a recent study that found a very high rate of stent thrombosis (21%) among patients with COVID-19 and STEMI. “I’m hoping that this will increase awareness [that] will change how we manage [COVID-19] patients after they get a stent: what choice of antiplatelets and anticoagulants to use for those particular types of patients,” the lead researcher told Cox.
TCTMD’s Caitlin Cox reports on a recent study that found a very high rate of stent thrombosis (21%) among patients with COVID-19 and STEMI. “I’m hoping that this will increase awareness [that] will change how we manage [COVID-19] patients after they get a stent: what choice of antiplatelets and anticoagulants to use for those particular types of patients,” the lead researcher told Cox.
Older, critically ill patients with COVID-19 treated with the antiretroviral drugs lopinavir and ritonavir appear to have a greater risk of bradycardia, a study in Circulation: Arrhythmia and Electrophysiology indicates. “Intensivists should be aware of this potential side effect in order to closely monitor lopinavir/ritonavir plasma levels, notably in elderly patients,” the authors say.
Screening conventional COVID-19 symptoms or signs of febrile respiratory illness may not be sufficient for identifying COVID-19 patients in the prehospital emergency setting, a study in JAMA Network Open suggests. “The findings have potential implications for early identification of COVID-19 and effective strategies to mitigate infectious risk during emergency care.”
International regulators under the umbrella of the International Coalition of Medicines Regulatory Authorities (ICMRA), including the US Food and Drug Administration (FDA) and the European Medicines Agency (EMA), have released their positions on the data needed to support moving into phase III vaccine trials and considerations for the design of those trials.
In a conversation with US National Institutes of Health (NIH) Director Francis Collins, MD, PhD, the researcher leading the agency’s COVID-19 vaccine effort said “an optimistic scenario would be that we get an answer in the phase III trial towards the end of this year. We have scaled up the production in parallel, so the vaccine should be available in great supply. We still must allow for the FDA to review the data and be comfortable with licensing the vaccine. Then we must factor in a little time for distributing and recommending that people get the vaccine.”
 Sweden’s decision to largely carry on rather than implement lockdowns in the face of COVID-19 has not turned out well, according to a story in the New York Times that says the country has become the “world’s cautionary tale.” Why is that? “Not only have thousands more people died than in neighboring countries that imposed lockdowns, but Sweden’s economy has fared little better.”
Sweden’s decision to largely carry on rather than implement lockdowns in the face of COVID-19 has not turned out well, according to a story in the New York Times that says the country has become the “world’s cautionary tale.” Why is that? “Not only have thousands more people died than in neighboring countries that imposed lockdowns, but Sweden’s economy has fared little better.”
Researchers have highlighted the potential for COVID-19-related brain damage in a study in Brain. The senior author of the study told Reuters: “Whether we will see an epidemic on a large scale of brain damage linked to the pandemic—perhaps similar to the encephalitis lethargica outbreak in the 1920s and 1930s after the 1918 influenza pandemic—remains to be seen.”
A JAMA research letter shows that COVID-19 case rates have been higher and rising faster in prisons than in the general US population, suggesting that more effective infection control measures are needed to stem the spread of SARS-CoV-2 in such facilities.
Also in JAMA, Tyler VanderWeele, PhD, discusses the challenges of estimating total lives lost during the COVID-19 pandemic and the impact of various policy decisions: “In the months ahead, while confronting the possibility of a second wave of the pandemic, these calculations of total lives lost, both from SARS-CoV-2 infection and because of social, psychological, and unemployment outcomes, may prove important in policy decisions.”
Holder pasteurization effectively inactivates SARS-CoV-2 in donated human milk, a study in CMAJ affirms. “Thus, in the event that donated human milk contains SARS-CoV-2 by transmission through the mammary gland or by contamination, this method of pasteurization renders milk safe for consumption and handling by care providers,” the authors conclude.
 College sports will not look the same in the fall due to COVID-19. Stanford University permanently cut 11 sports to help offset a projected $70 million shortfall over the next 3 years, partly related to the pandemic. And the Ivy League has decided that there will be no fall sports at its institutions in 2020.
College sports will not look the same in the fall due to COVID-19. Stanford University permanently cut 11 sports to help offset a projected $70 million shortfall over the next 3 years, partly related to the pandemic. And the Ivy League has decided that there will be no fall sports at its institutions in 2020.
July 8, 2020
The US federal government will set up new temporary testing sites in three states—Florida, Louisiana, and Texas—that are seeing ballooning numbers of COVID-19 cases, Bloomberg reports. Deaths are rising in Texas, while the median age of cases has gone up in Florida. One expert quoted in the story noted that an increase in deaths is inevitable after a surge in cases. “We are in the calm before the storm,” she said.
 A news story in Science delves into what’s known about how to limit the spread of SARS-CoV-2 when reopening schools. Experts fear that long-term school closures will have lingering detrimental effects on children. There are limited data on what measures work best to stem transmission when sending kids back into classrooms, but the experiences of other countries “suggest a combination of keeping student groups small and requiring masks and some social distancing helps keep schools and communities safe, and that younger children rarely spread the virus to one another or bring it home.”
A news story in Science delves into what’s known about how to limit the spread of SARS-CoV-2 when reopening schools. Experts fear that long-term school closures will have lingering detrimental effects on children. There are limited data on what measures work best to stem transmission when sending kids back into classrooms, but the experiences of other countries “suggest a combination of keeping student groups small and requiring masks and some social distancing helps keep schools and communities safe, and that younger children rarely spread the virus to one another or bring it home.”
A European Society of Cardiology (ESC) podcast focuses on a recent study that looked at the impact of the COVID-19-related lockdown on the outcomes of patients with new-onset A-fib in Denmark. The study authors conclude: “In the event of prolonged or subsequent lockdowns, the risk of undiagnosed AF patients developing complications could potentially translate into poorer outcomes in patients with AF during the COVID-19 pandemic.”
A research letter in JAMA Cardiology describes a patient with COVID-19 who developed late stent thrombosis after DES implantation. Though the event could not be directly linked to COVID-19, “these findings suggest that special care should be paid to optimize antithrombotic therapy in patients with COVID-19 with previous coronary artery disease,” the authors say.
Writing in STAT, a third-year psychiatry resident at NewYork-Presbyterian Hospital says his COVID-19 symptoms have lasted for more than 100 days, and he points out that there are others who have experienced the same thing. “As we enter the next phase, increasing evidence points to a significant proportion of us with prolonged symptoms, and this warrants attention,” he writes, linking to a prior story in The Atlantic on COVID-19 “long-haulers.”
 The next installment of the American College of Cardiology’s free Summer COVID-19 Education Series will address how to safely return to organized sports and exercise. The session will take place from 12 to 1 pm ET on Thursday, July 9.
The next installment of the American College of Cardiology’s free Summer COVID-19 Education Series will address how to safely return to organized sports and exercise. The session will take place from 12 to 1 pm ET on Thursday, July 9.
With increasing evidence that SARS-CoV-2 may be more easily transmittable through the air than previously thought, Apoorva Mandavilli of the New York Times asks: what should you do now? Authors of an open letter to the World Health Organization (WHO) say that “people should consider minimizing time indoors with people outside their families,” according to the story. “Schools, nursing homes, and businesses should consider adding powerful new air filters and ultraviolet lights that can kill airborne viruses.” Wearing masks remains important.
The US National Institute of Allergy and Infectious Diseases (NIAID) has launched a clinical trials network to test vaccines and monoclonal antibodies to protect against COVID-19, according to a press release. The COVID-19 Prevention Trials Network merges four existing networks across the country.
The vast majority of workers in US meat and poultry processing facilities who have developed COVID-19 (87%) belong to racial/ethnic minority groups, according to a study in Morbidity and Mortality Weekly Report. “Targeted workplace interventions and prevention efforts that are appropriately tailored to the groups most affected by COVID-19 are critical to reducing both COVID-19–associated occupational risk and health disparities among vulnerable populations,” the authors say.
July 7, 2020
The United States is nearing 3 million confirmed COVID-19 cases, among more than 11.6 million worldwide, according to the Johns Hopkins COVID-19 Dashboard. At least 130,000 Americans have died from the disease. Parts of the US, particularly in the South and West, are continuing to see surging case numbers.
Anthony Fauci, MD, director of the US National Institute of Allergy and Infectious Diseases, said Monday that the average age of COVID-19 patients has fallen by about 15 years over the past few months, as CNBC reports. He also characterized the recent increase in cases as a continuation of the initial SARS-CoV-2 outbreak and not a second wave.
New data out of Italy are consistent with most prior studies in showing that antihypertensive medications, including ACE inhibitors, ARBs, and calcium channel blockers, do not influence prognosis in patients with COVID-19.
Venous thromboembolism is not more common in patients with COVID-19 pneumonia versus community-acquired pneumonia, according to a study in Arteriosclerosis, Thrombosis, and Vascular Biology.
Two JAMA viewpoints tackle the rapid development of vaccines for SARS-CoV-2. One describes the different types of vaccine candidates, and the other stresses that safeguards are needed to ensure that any vaccine that emerges is safe and effective so the public has trust in its use.
 According to Reuters, the World Health Organization (WHO) is reviewing the open letter written by 239 scientists that asks the agency to update its guidance to better reflect the potential for airborne spread of SARS-CoV-2.
According to Reuters, the World Health Organization (WHO) is reviewing the open letter written by 239 scientists that asks the agency to update its guidance to better reflect the potential for airborne spread of SARS-CoV-2.
A survey study published as a preprint in the American Journal of Gastroenterology indicates that people who use proton pump inhibitors (PPIs) are more likely to report a positive COVID-19 test compared with nonusers. “Further studies examining the association between PPIs and COVID-19 and whether they increase the risk for more severe disease are needed,” the authors say.
 The US Food and Drug Administration (FDA) has updated its guidance on how to conduct trials during the pandemic, adding information on obtaining informed consent and clarifying recommendations on documentation when using video conferencing for study visits.
The US Food and Drug Administration (FDA) has updated its guidance on how to conduct trials during the pandemic, adding information on obtaining informed consent and clarifying recommendations on documentation when using video conferencing for study visits.
The agency also sent a letter to clinical laboratory staff and healthcare professionals about the increased risk of false-positive results when using BD SARS-CoV-2 Reagents for the BD Max System diagnostic test. One study showed a roughly 3% false-positive rate using that test.
A modeling study in PNAS suggests that even if all symptomatic people with COVID-19 are isolated, that might not be enough to prevent outbreaks due to spread by either presymptomatic or asymptomatic infections. “Our results indicate that symptom-based isolation must be supplemented by rapid contact tracing and testing that identifies asymptomatic and presymptomatic cases, in order to safely lift current restrictions and minimize the risk of resurgence,” they conclude.
July 6, 2020
A study in the American Journal of Cardiology describes the characteristics and outcomes of patients presenting with COVID-19 and STEMI at four hospitals in Italy, Lithuania, Spain, and Iraq. Most (76%) were treated with fibrinolysis, with the rest undergoing primary PCI. Stent thrombosis occurred at a very high rate (21%), “indicating a possible need to adapt STEMI management for COVID-19 patients,” the authors say.
 In an open letter to the World Health Organization (WHO), 239 scientists claim that the agency is downplaying the risk of airborne spread of SARS-CoV-2, as the New York Times reports.
In an open letter to the World Health Organization (WHO), 239 scientists claim that the agency is downplaying the risk of airborne spread of SARS-CoV-2, as the New York Times reports.
Meanwhile, the WHO has discontinued the hydroxychloroquine and lopinavir/ritonavir treatment arms of its Solidarity trial looking into treatments in hospitalized COVID-19 patients. Preliminary results show the regimens “produce little or no reduction in the mortality of hospitalized COVID-19 patients when compared to standard of care.”
A research letter in JAMA Internal Medicine illustrates the early enthusiasm around hydroxychloroquine and chloroquine, showing spikes in outpatient prescriptions for the drugs in February and March as the SARS-CoV-2 outbreak was gaining steam in the United States.
In the American Heart Journal, D. Edmund Anstey, MD, and colleagues describe the changes made to the cardiac intensive care unit (CICU) at their center in New York City and the evolving role of critical care cardiologists and other clinicians during the pandemic. “Cardiac intensivists should anticipate being the primary clinician for many COVID-19 positive patients,” they write. “Further, the CICU intensivist must be mindful of the large team of clinicians who will similarly face complex and novel challenges with COVID-19, including nurses, advanced practice providers, pharmacists, respiratory therapists, physical therapists, and social workers, among others.”
 Findings from a preprint study show that a segment of DNA associated with more-severe COVID-19 was passed down from Neanderthals about 60,000 years ago, Carl Zimmer reports in the New York Times.
Findings from a preprint study show that a segment of DNA associated with more-severe COVID-19 was passed down from Neanderthals about 60,000 years ago, Carl Zimmer reports in the New York Times.
The potential implications in terms of cardiac arrhythmia related to prophylactic use of hydroxychloroquine/chloroquine are discussed in a new review in Heart Rhythm. Because of the potential risks, ongoing ECG monitoring is recommended.
The University of Chicago’s US COVID Atlas provides an interactive look at regional and county-level data to provide near real-time insights into the ongoing pandemic and how it’s changing over time.
July 3, 2020

“I think it’s pretty obvious that we’re not going in the right direction,” Anthony S. Fauci, MD, said in conversation with JAMA editor-in-chief Howard Bauchner, MD, as part of the JAMA website’s COVID-19 Q&A video series. “There is no blame here, there’s none of that: we need to realize that if we do not adhere to the guidelines as we’re trying to open up . . . we’re going to be in some serious difficulty. Right now if you look at the number of cases, it’s quite disturbing. We’re setting records practically every day for new cases.”
Flying in the face of other recent research, an observational study performed at six hospitals in the Henry Ford Health System (HFHS) and published in the International Journal of Infectious Diseases concludes that hydroxychloroquine alone or in combination with azithromycin may reduce COVID-19 associated mortality. Twitter has erupted in condemnation of the study. A tweetorial by David Cohen, MD, explains why.
The US Food and Drug Administration is warning consumers not to use sanitizer products that contain methanol, which is often used in fuels and antifreeze. “Methanol is not an acceptable active ingredient for hand sanitizer products and can be toxic when absorbed through the skin as well as life-threatening when ingested,” the agency warns. In other news, the FDA has also issued an emergency use authorization for a third diagnostic test that can detect and differentiate between influenza and COVID-19.
The number of patients presenting to hospital with acute ischemic stroke during the pandemic is higher than that seen in patients ill with influenza during the same time window in previous years. “Additional studies are needed to confirm these findings and to investigate possible thrombotic mechanisms associated with COVID-19,” Alexander E. Merkler, MD, and colleagues write in JAMA Neurology.
A phase 3, randomized, placebo-controlled trial of an RNA-based vaccine against COVID-19 has been delayed, STAT news reports. Changes to the study protocol mean the first patients in what has been designed as a 30,000-patient trial will not get the drug, mRNA-1273, on July 9 as initially intended, although one investigator has said he believes the manufacturer, Moderna, is still aiming to start the trial this month.
 There’s a whiff of good news from JAMA Otolaryngology–Head & Neck Surgery: a prospective study out of Italy suggests that 89% of people who had sudden onset loss of smell or taste “experienced a complete resolution or improvement of these symptoms,” after 4 weeks. In the same journal, Brooke M. Su-Velez, MD, PhD, and colleagues offer recommendations for safely decontaminating and reusing N95 respirators concluding “there are several options for institutions to consider for both immediate and large-scale implementation.”
There’s a whiff of good news from JAMA Otolaryngology–Head & Neck Surgery: a prospective study out of Italy suggests that 89% of people who had sudden onset loss of smell or taste “experienced a complete resolution or improvement of these symptoms,” after 4 weeks. In the same journal, Brooke M. Su-Velez, MD, PhD, and colleagues offer recommendations for safely decontaminating and reusing N95 respirators concluding “there are several options for institutions to consider for both immediate and large-scale implementation.”
The complex needs of patients with psychiatric conditions pose special problems for high-risk residential facilities admitting new patients. Healthcare professionals at a facility in Wyoming describe the enhanced procedures they put in place when admitting two patients with SARS-CoV-2 infection, managing to successfully limit any spread of the contagion. Every day, approximately 180,000 patients in the United States seek out mental health services from one of approximately 4,000 inpatient and residential psychiatric facilities, the authors note.
The National Institutes of Health website has posted the witness testimony of Francis Collins, MD, PhD, Robert R Redfield, MD, and Gary Disbrow, PhD, to the Senate Appropriations Committee Subcommittee on Labor, Health and Human Services, Education, and Related Agencies about progress to date in the federally funded “Operation Warp Speed,” aimed at the rapid development and commercialization of an effective COVID-19 vaccine. “We’re putting billions of dollars on the line to solve a multi-trillion-dollar challenge,” the testimony reads. Writing in Science, Jon Cohen reports that the three men, who head up different branches of the Department of Health and Human Services, managed to evade questions on which vaccines are the current focus of the project, citing procurement processes and market forces as reasons for their obfuscation.
Left ventricular global longitudinal strain (GLS) on echocardiography appears to be a predictor of mortality in hospitalized patients with COVID-19, investigators report in the American Journal of Cardiology. In the small, single health center study from Cleveland, each 1% increase in GLS was associated with increased mortality, a finding that persisted after adjustments for age and LV ejection fraction.
An American Heart Association statement says that its leadership is “deeply troubled” by efforts to undermine the expertise and authority of public health officials trying to protect patients and champion health during the COVID-19 pandemic. “Public health officials deserve our thanks and support for their efforts to respond to this historic pandemic,” the statement reads. “What they do not deserve are threats of personal harm, attacks on their professional integrity or pressure in any form to cease speaking to the best available science.”

Contributed today by Shelley Wood.
July 2, 2020 During the 8-week period between March 1 to April 25 of this year, there were an estimated 87,001 excess deaths in the United States, of which about two-thirds were attributed to COVID-19, researchers report in a JAMA research letter. “Large increases in mortality from heart disease, diabetes, and other diseases were observed,” they note. “Further investigation is required to determine the extent to which these trends represent nonrespiratory manifestations of COVID-19 or secondary pandemic mortality caused by disruptions in society that diminished or delayed access to health care and the social determinants of health (eg, jobs, income, food security).” Listen to an author interview here.
During the 8-week period between March 1 to April 25 of this year, there were an estimated 87,001 excess deaths in the United States, of which about two-thirds were attributed to COVID-19, researchers report in a JAMA research letter. “Large increases in mortality from heart disease, diabetes, and other diseases were observed,” they note. “Further investigation is required to determine the extent to which these trends represent nonrespiratory manifestations of COVID-19 or secondary pandemic mortality caused by disruptions in society that diminished or delayed access to health care and the social determinants of health (eg, jobs, income, food security).” Listen to an author interview here.
COVID-19-related lockdowns were associated with a 32% reduction in endovascular procedures for acute ischemic stroke and an estimated 54-minute increase in symptom onset-to-groin puncture time, a study of centers in Europe and North America, published in Stroke, shows.
A systematic review and meta-analysis evaluating the diagnostic accuracy of serological tests for COVID-19 shows that lateral-flow immunoassays, which are used at the point of care, are less sensitive than other assays, although the authors, writing in the BMJ, conclude that higher-quality studies are needed.
 SARS-CoV-2 may have been circulating in New York City, where the first confirmed COVID-19 case was identified on February 29, as early as the beginning of that month, according to a preprint article. The findings are strengthened by their consistency with other research, the New York Times reports.
SARS-CoV-2 may have been circulating in New York City, where the first confirmed COVID-19 case was identified on February 29, as early as the beginning of that month, according to a preprint article. The findings are strengthened by their consistency with other research, the New York Times reports.
Obesity is associated with a relative 39% increase in the odds of critical illness—defined as death or a need for ICU care, invasive mechanical ventilation, or hospice care—among patients hospitalized with COVID-19, according to a study in Mayo Clinic Proceedings. The researchers call this a “worrisome sign” considering the high prevalence of overweight and obesity around the world.
Survey results in JAMA Network Open show that people in China often reported symptoms of depression (27.9%), anxiety (31.6%), insomnia (29.2%), and acute stress (24.4%) during the pandemic. Those with confirmed/suspected COVID-19 and their family members and friends, as well as people with occupational exposure risks, were particularly at risk for having these symptoms.
A study of 27 children with COVID-19 pediatric multisystem inflammatory syndrome showed that four (14.8%) who were previously healthy had new-onset neurological symptoms, including encephalopathy, headaches, brainstem and cerebellar signs, muscle weakness, and reduced reflexes. All required intensive care, researchers report in JAMA Neurology.

“Repeated point prevalence surveys in skilled nursing facilities can identify asymptomatic COVID-19 cases, inform cohorting and infection prevention and control practices, and guide prioritization of health department resources,” researchers conclude in Morbidity and Mortality Weekly Report after analyzing the results of such an approach in 26 facilities in Detroit.
NEW—Individual decisions to reduce movement – even before state-wide stay-at-home policies were introduced – likely helped slow the spread of #COVID19 in the USA: finding from a mathematical modelling study with mobile phone data @TheLancetInfDis https://t.co/VEONXZfVuC pic.twitter.com/mWCJMQD4Dq
— The Lancet (@TheLancet) July 1, 2020
A look at how people were moving around in the United States from January 1 to April 20 based on cell phone data, published in the Lancet Infectious Diseases, supports social distancing as an effective way to slow spread of SARS-CoV-2. The study also shows that Americans were starting to change their behaviors even before stay-at-home orders were issued.Patient and public involvement, left out of decision-making in the early days of the COVID-19 pandemic, need to be brought back, according to an editorial in the BMJ. “COVID-19 has precipitated a global health crisis, plunged the world into economic recession, put the spotlight on structural inequalities, including racism, and galvanized the call for action on climate change,” the authors write. “The knowledge to confront these challenges needs to be coproduced. Patient and public involvement must be taken seriously, embedded robustly, and never sidelined again.”
Patient and public involvement, left out of decision-making in the early days of the COVID-19 pandemic, need to be brought back, according to an editorial in the BMJ. “COVID-19 has precipitated a global health crisis, plunged the world into economic recession, put the spotlight on structural inequalities, including racism, and galvanized the call for action on climate change,” the authors write. “The knowledge to confront these challenges needs to be coproduced. Patient and public involvement must be taken seriously, embedded robustly, and never sidelined again.”
July 1, 2020
As the United States saw its biggest 1-day spike in new COVID-19 cases on Tuesday (more than 47,000), Anthony Fauci, MD, director of the US National Institute of Allergy and Infectious Diseases, told a Senate committee, “Clearly we are not in total control right now,” as reported by Reuters. The daily increase in new cases could reach 100,000 if more is not done to control spread of the virus, he said: “We can’t just focus on those areas that are having the surge. It puts the entire country at risk.”
 Adding to the concern around COVID-19 are reports that a new strain of H1N1 swine flu, possessing what is called a G4 genotype, is spreading to humans in China. In a PNAS study, researchers state that “G4 viruses have all the essential hallmarks of a candidate pandemic virus. Of concern is that swine workers show elevated seroprevalence for G4 virus. Controlling the prevailing G4 EA H1N1 viruses in pigs and close monitoring in human populations, especially the workers in swine industry, should be urgently implemented.”
Adding to the concern around COVID-19 are reports that a new strain of H1N1 swine flu, possessing what is called a G4 genotype, is spreading to humans in China. In a PNAS study, researchers state that “G4 viruses have all the essential hallmarks of a candidate pandemic virus. Of concern is that swine workers show elevated seroprevalence for G4 virus. Controlling the prevailing G4 EA H1N1 viruses in pigs and close monitoring in human populations, especially the workers in swine industry, should be urgently implemented.”
The United States has bought up nearly the entire supply of the investigational antiviral remdesivir (Gilead Sciences) expected to be produced through September, leaving little for the rest of the world. According to the Department of Health and Human Services (HHS), the 500,000 treatment courses that will be made available to US hospitals represents all of the projected production for July and 90% of the expected production in August and September.
In the Journal of the American Heart Association, researchers from Wuhan, China, report that age over 70 and elevations of C-reactive protein, lactate dehydrogenase, and lactic acid were independent risk factors for myocardial damage in patients hospitalized with COVID-19.
A perspective from the Agency for Healthcare Research and Quality’s (AHRQ) Patient Safety Network states that the COVID-19 pandemic, and the healthcare system’s response to it, has presented challenges to ensuring medication safety. Those difficulties are related to “medication shortages, changes to the pharmacy workflow, an ever-changing evidence base associated with the pharmaceutical treatment of COVID-19 complications, and limited availability of personal protective equipment (PPE).”
 On Tuesday, the US Food and Drug Administration (FDA) issued guidance for industry around the development and licensure of COVID-19 vaccines. Of note, the agency says that to ensure effectiveness, the point estimate for efficacy in a placebo-controlled trial should be at least 50%.
On Tuesday, the US Food and Drug Administration (FDA) issued guidance for industry around the development and licensure of COVID-19 vaccines. Of note, the agency says that to ensure effectiveness, the point estimate for efficacy in a placebo-controlled trial should be at least 50%.
A study in the Lancet Public Health shows that disease outcomes among adult patients hospitalized with COVID-19 are better predicted by frailty—assessed using the clinical frailty scale (CFS)—than by age or comorbidities.
In the next installment of the American College of Cardiology’s free Summer COVID-19 Education Series, John Erwin III, MD, will moderate a discussion about how clinicians can improve their overall wellness and mental well-being during the pandemic. The session will take place from 12 to 1 pm ET on Thursday, July 2.
In Morbidity and Mortality Weekly Report, results of a survey of adult inpatients and outpatients who tested positive for SARS-CoV-2 show that only 46% reported recent contact with a COVID-19 patient. “Case investigation, contact tracing, and isolation of infected persons are needed to prevent ongoing community transmission, given the frequent lack of a known contact,” the authors say.
 The European Union is reopening its borders to visitors from 15 countries, but the United States is not on the list, the New York Times reports.
The European Union is reopening its borders to visitors from 15 countries, but the United States is not on the list, the New York Times reports.
COVID-19: TCTMD's Daily Dispatch for September
COVID-19: TCTMD’s Daily Dispatch for August
COVID-19: TCTMD’s Daily Dispatch for June
COVID-19: TCTMD’s Daily Dispatch for May
COVID-19: TCTMD’s Daily Dispatch for April
COVID-19: TCTMD’s Daily Dispatch for March
Todd Neale is the Associate News Editor for TCTMD and a Senior Medical Journalist. He got his start in journalism at …
Read Full Bio

Comments